Medical research is often a slow, incremental, iterative process. Breakthroughs come about in many cases because of the small contributions of many research groups, each helping to solve critical pieces of the puzzle.
Such was the case in January with a groundbreaking operation at the University of Maryland. The operation called for transplanting a genetically modified pig heart into a 57-year-old man in a last-ditch effort to save his life. It was the first time a pig’s heart was successfully transplanted into a human being. After not immediately rejecting the heart, a common occurrence in transplantation procedures, the patient lived for two months before passing away on March 8.
This is called xenotransplant technology, which refers to transplanting organs between species – in this case, pig and human.

While working more than 20 years ago at the Nashville VA, Dr. Richard Pierson studied a new method of immunosuppression using heart transplants from genetically modified pigs in baboons. The research served as a “proof of principle” for eventual application to humans.
‘All of us felt inspired’
VA-funded research starting in the 1990s helped uncover knowledge that proved to be key – along with findings by many other groups – to establishing the technique of transplanting a pig’s heart into a person. The researcher leading this work at VA was Dr. Richard Pierson, a specialist in thoracic and cardiac surgery who is now with Massachusetts General Hospital and Harvard University.
While at the Nashville VA Medical Center in Tennessee from 1994 to 2002, Pierson received funding from VA’s Office of Research and Development to study how to alter the immune system in baboon recipients of genetically modified pig hearts so the heart would not be rejected. This research, he says, was a “proof of principle” intended for eventual application to humans. The pioneering work earned him further funding and recognition with a VA Merit Award in 1998 and a Presidential Early Career Award for Scientists and Engineers (PECASE) in 1999, both of which he used to advance his research.
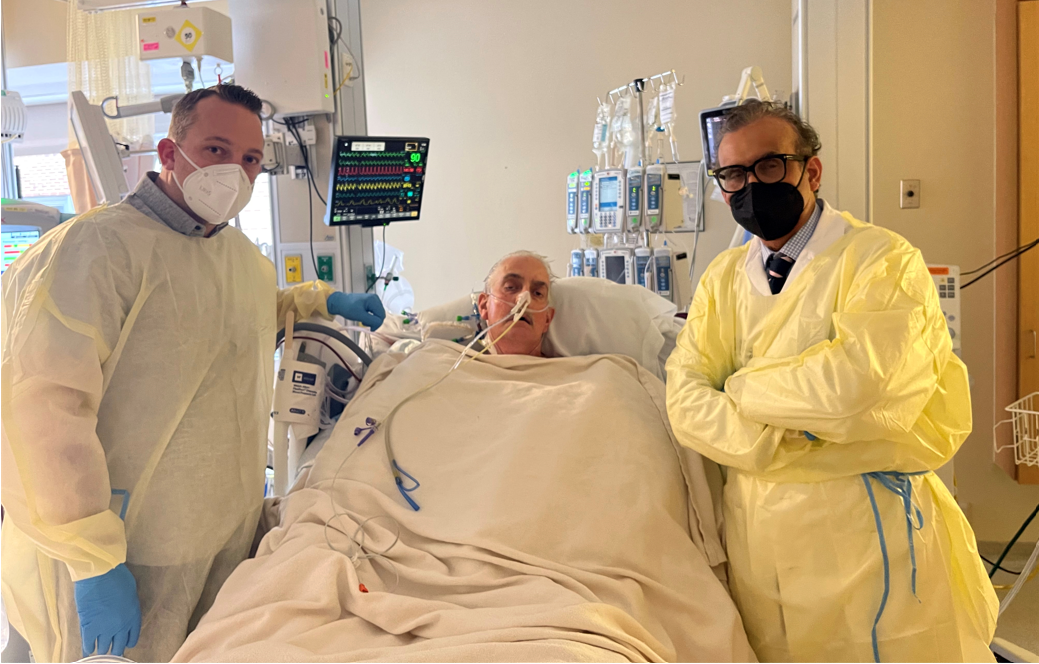
Pierson was thrilled to hear about the successful transplant at the University of Maryland, where he carried out research on xenotransplantation for about 15 years. Dr. Muhammad Mohiuddin, whom Pierson has collaborated with on studies of transplanting animal organs into humans, was one of the lead surgeons on the Maryland team.
“All of us felt inspired that someone had taken this step, and that it had been successful,” Pierson says. “Many of us would have predicted that a heart with genetic modifications probably would be able to function relatively normally in a human, but that’s a different thing than proving it can actually happen. This transplant was historic.”
Surgery took years to pull off
That the patient, David Bennett, lived for two months supported by a pig’s heart is remarkable, Pierson says, although he’s disappointed that Bennett didn’t live for years.
“Those of us who are advocates for this basic technology hope the heart and patient are going to live for a long time every time we do a transplant,” he says. “The longest that non-human primates have been supported with an orthotopic heart transplant has been six or eight months. But those experiments in many instances have been limited by regulatory decisions to stop the experiment, as in the German experience, or by logistical problems with it being expensive and complicated to take care of an animal with a heart transplant. I’m confident that with the right pig, the right treatments, and the right patient, we really could make this work with what we know today.”
Dr. David Klassen, chief medical officer of the United Network for Organ Sharing, says it took years of basic research by many scientists to pull off the surgery on Bennett.
“Despite his death, this transplant remains an important step toward making xenotransplants possible for patients in need of a heart transplant,” Klassen says. “This ought to remind us of the complexity of these approaches and the many challenges that will remain before these therapies can be developed and widely applied. I’m confident a lot will be learned from this transplant even though it was only one transplant.”
More Information
Click here to read the full story.
Click here to learn more about VA research.
Topics in this story
More Stories
Diverse representation of women in health care research allows MVP to make discoveries for women’s health
Join the Million Veteran Program online. You will have the option to receive an at-home blood sample collection kit in the mail.
VHA's new podcast series, New Horizons in Health, features a candid discussion of psychedelic assisted therapies for Veterans experiencing mental health conditions.