U.S. Army Veteran, Sunsara Smith, spent seven years waking up each night with a burning sensation in her throat thanks to acid reflux.
“My doctors tried several different things, but nothing worked,” said Smith.
Nightly sleep interruptions, thanks to acid reflux or Gastroesophageal reflux disease, (GERD) is a reality for thousands of Veterans. To remedy this, several VA North Texas physicians coordinated and collaborated with VA medical centers from across the country on a multi-year study to determine the most effective treatment protocols. The authors published their results in the preeminent New England Journal of Medicine.
“It’s very exciting to know that we’re a part of making our profession of medicine better, not just for our Veterans, but for everyone,” said Dr. Thai Pham, VA North Texas lead surgeon on the study who specializes in upper-GI procedures.
A simple, surgical solution

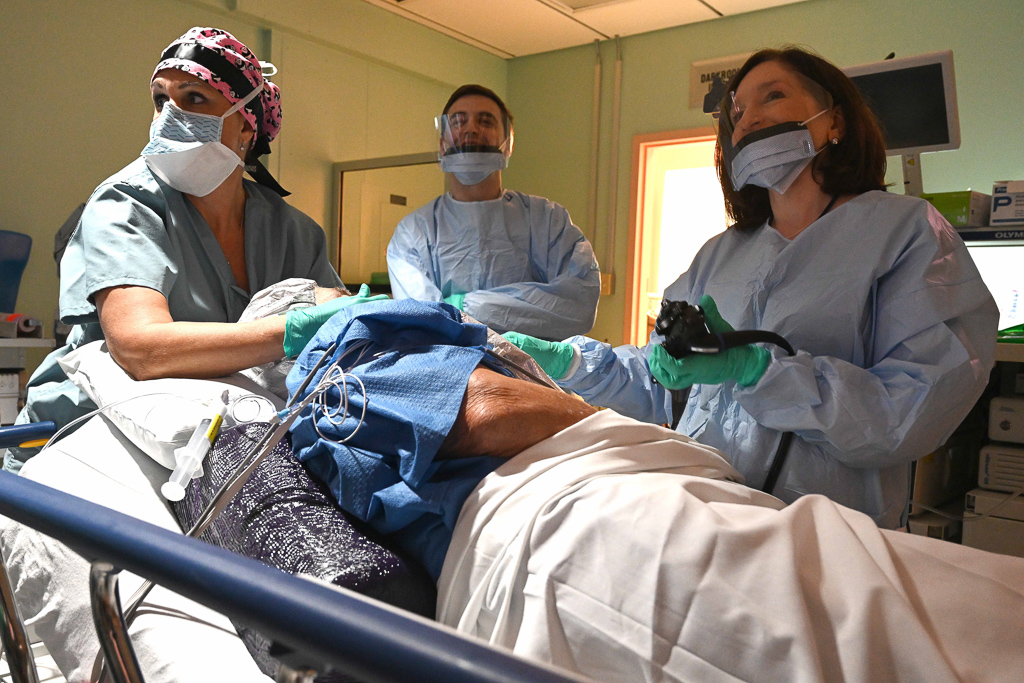
Dr. Shelby Melton, senior pathologist at VA North Texas Health Care System examines a tissue sample to help determine the condition a Veteran is suffering from. Dr. Melton was recently honored as part of a team of doctors to have a paper published in the New England Journal of Medicine chronicling the results of a study conducted as part of the VA Cooperative Studies Program having to do with the evaluation and treatment of Gastroesophageal reflux disease (GERD) – A digestive disorder that affects the ring of muscle between the esophagus and stomach. Many people, including pregnant women, suffer from heartburn or acid indigestion caused by GERD.
GERD is a digestive disorder that affects the lower esophageal valve that controls the flow between the esophagus and stomach. Many people, including pregnant women, suffer from heartburn or acid indigestion caused by GERD. Smith worked with her medical team for years before moving to the Dallas area. That’s where she met Pham, and her evaluation led to a simple, yet effective, surgical solution to her heartburn.
The study concluded that a relatively simple surgical procedure can end the suffering for many afflicted with chronic heartburn.
“This was the first head-to-head study of this nature,” said Dr. Kerry Dunbar, section chief for VA North Texas Gastroenterology and lead gastroenterologist on the study. “And it was only possible because of the VA’s ability to collaborate nationally.”
The study took an in-depth look at the common treatments and protocols of chronic heartburn to determine the best medical treatment. They evaluated nearly 400 patients from 13 VA medical centers from across the country. The results show that nearly 70% of patients benefited from a surgery called Nissen fundoplication, or Lap Nissen. Lap Nissen, or keyhole surgery, is a minimally invasive procedure that requires several tiny incisions to perform and has patients back on their feet within hours.
“I can sleep through the night now.”
VA North Texas evaluated Smith using the protocols and procedures established in the study. Her care team determined she was a good candidate for the Lap Nissen surgery, which she underwent several weeks ago.
“Its been two weeks and I’m able to sleep through the night now,” said Smith. “The doctors and nurses have been great – they took the time to really understand what was going on with me.”
Veterans that participated in the study were evaluated through a vigorous series of medical protocols coordinated across the country by the Dallas team. All of the results were sent back to the study team at the Dallas VAMC. The study’s outcomes show broader impacts in treating chronic heartburn, beyond validating the efficacy of a surgical solution. Several outcomes derived from the study will go on to help patients with chronic heartburn through better medication management and evaluation protocols.
Veterans that fit the initial study parameters, which included ongoing medical treatment using protein pump inhibitor medications to stop the body’s production of stomach acids, were evaluated and their current medication treatment closely monitored. The study found that for many of the patients–more than 12 percent– that taking their medications precisely as directed, 30-minutes prior to eating, resolved their heart burn.
“It was great to be an investigator for this study,” said Dunbar. “It demonstrates the outstanding research that can be accomplished when VA sites collaborate.”
National collaboration, multiple beneficial outcomes
Another beneficial outcome of the study deals directly with how causes of the chronic heartburn is evaluated by providers. The study demonstrated that many Veterans benefited from simple life style changes, precluding the need for daily medications or even surgery.
Throughout the Veterans Health Administration (VHA), many dedicated researchers are working to improve the health and health care of Veterans. From research on tuberculosis in the 1940s to today’s developments in advanced robotic prosthetics, the Department of Veterans Affairs (VA) has ranked as one of the nation’s leaders in health research.
“Most importantly, this achievement validates the hard work done and cutting-edge research performed by VA staff in support of our Veterans,” commented Dr. Shelby Melton, leading pathologist on the study. “The sharing of this groundbreaking study by the most reputable medical journal demonstrates how VHA is working to provide the best possible health care to our Veterans, while contributing to better health practices for all.”
Michael Cole is a public affairs specialist with VA North Texas Health Care System.
Topics in this story
More Stories
Diverse representation of women in health care research allows MVP to make discoveries for women’s health
Join the Million Veteran Program online. You will have the option to receive an at-home blood sample collection kit in the mail.
VHA's new podcast series, New Horizons in Health, features a candid discussion of psychedelic assisted therapies for Veterans experiencing mental health conditions.






The Nissan fundoplication helped me really well from 2010 til about 2017. Then it came back with a vengeance! At that point we found more hernias and that the Nissan area opened up and formed a pocket. The last time they decided on a gastric bypass to help. And yes, they still want me to take a medication, but it has really helped. It was done in Sept 2017.
Jen, Thank you for your comments and I’m sorry you suffer with this. I hope your docs can find the right answer for you.
“Its been two weeks and I’m able to sleep through the night now,” said Smith.
So it would appear the operation was a success!
I just want to know where to sign up to get it!!!!1
You never said whether or not Sunsara Smith is free of GERD medications post surgery.
Rodney, Good point. So far, yes she’s doing well.
As a Veteran who has suffered from this on a daily and nightly basis for years, I am excited to see what’s being done to help. It’s not just an occasional bout of heartburn. GERD is chronic and makes it tough to experience a restful night.