VA Geriatric Scholar Jessica Alva was a neuropsychologist at Central Virginia VA when her clinic quickly shifted to telehealth during the pandemic. With this change she noticed a large discrepancy among older Veterans’ use of VA Video Connect (VVC) compared to other age groups.
“Seventy-five percent of our older Veterans were unable to complete a telehealth visit due to a lack of equipment or low technology literacy,” said Alva.
Motivated by her recent training with the VA Geriatric Scholars Program, she launched a quality improvement project to help older Veterans reap the benefits of VA Video Connect. She collaborated with providers from the Central Virginia VA Geriatric Evaluation Clinic, a specialty team that is dedicated to comprehensive assessments of older Veterans with multiple medical and functional problems with the goal of optimizing health and daily function.
Proactively helping Veterans prepare for their telehealth visit
Alva’s team identified a major roadblock hindering the success of telehealth visits with VVC was that problems with technology or connectivity were not known until the actual telehealth appointment time, potentially leading to delays in needed health care.
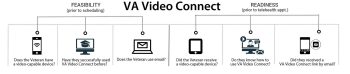 The team decided they could solve most issues proactively by gathering key information while engaging with the patient at two different time points. First, to assess if it was feasible for the older Veteran to engage in a telehealth visit, then to see if they were ready for that visit.
The team decided they could solve most issues proactively by gathering key information while engaging with the patient at two different time points. First, to assess if it was feasible for the older Veteran to engage in a telehealth visit, then to see if they were ready for that visit.
The information gathered determined specific needs the team could address. If the Veteran didn’t have a video-capable device, they arranged for the delivery of an iPad. If the Veteran had a device but was new to VA Video Connect, the team coordinated a test call to practice.
100% of older patients’ telehealth visits were successful
“It wasn’t a matter of figuring out how to address the barriers. It was a matter of identifying the main barriers in the first place,” said Alva. “Asking these focused questions allowed the team to quickly identify any potential problems and have enough time address them prior to the appointment.”
In just over two months, Veterans’ use of telehealth jumped to 47% from 29%. And 100% of scheduled telehealth appointments were completed successfully compared to 56% at the start of the project.
“Working as a team was critical in being able to make these positive changes. That combined effort makes change possible,” she added.
VA telehealth model of care benefits patients and providers
Dr. Alva’s neuropsychology and telehealth expertise unlocked new opportunities at VA. She recently joined the Veterans’ Cognitive Assessment and Management Program, or V-CAMP, at Greater Los Angeles VA. The V-CAMP team employs telehealth to increase access to cognitive evaluation, medication consultation, and care management for older Veterans in rural communities where access to dementia specialists is limited.
“V-CAMP serves Veterans who live hundreds of miles away, Veterans who might not be able to travel to the main VA Medical Center for a face-to-face appointment,” said Alva. She will remain in Virginia, now as a full-time remote neuropsychologist serving rural Veterans enrolled with Greater Los Angeles VA—evidence of the flexibility the VA telehealth model of care offers to patients and providers.
“It’s a perfect fit,” she said.
Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.







Perhaps some of the younger Vets could hep anyone needing help. Even I as a 73 year old with 53 years of marriage to my Vet would help anyone needing help.
I also need to mention- do you realize how much wives like me- struggle? We were engaged when he went to Nam. He was there 1968 & 1969. He was a Sargent but led troops as fellow “Ground Pounders”. He has his medals & even I —have no idea why he was given the Bronze Star! He is now 100% disabled & I have been there every step of the way. He came home in Sept of 1969 & we married in Nov 1969. He told me
“The war is over”. I love him with all my heart & will always be there for him. He has PTSD. He was too kind of a young man to NOT be effected by what he did & had to do to survive! Of course he gave a lot more than I— but sometimes I feel like what about me! What about what this did to our marriage ( very good) how much easier, happier& more fulfilling could it have been. We began our story at 16 & 18 years of age!
Please realize- it will never be over- until the day one of us passes ! It has affect our entire engaged & married life! It means constant living with “Waiting for the other shoe to fall”. With Agent Orange, UN recognized Burn Pits in Viet Nam, & the constant new “health & mental health issues- he has had to endure it but we both have LIVED IT. Now our only 2 Adult Children -conceived shortly AFTER NAM- have Autoimmune issues that do not “Run in our families”. Our Dear Daughter has Lupus, Schuerman’s Disease ( “Round Back Deformity”) AGAIN not a inherited problem & SHE HAS another immune problem. She CHOSE & Still works for “The Department of the Army” due to not being able to to find any other way- to Honor her beloved Father. Due to her health issues she chose NOT to Marry or have the kids we all dreamed of ! Our son has A.S. Anklyosising Spondolitis
( immunine & bone issue). Both of Our sons kids -have fingers /toes that are joined way beyond normal. $$ wise we are not asking for anything- I just want you to realize how much- THE WAR will never be over for our family. Not acknowledging the Burn Pits- for Viet Nam Vets -is crazy. You know that was a common practice for Constant Ground Pounders -that were on the move ! Why were they not included. My husband has always said next to nothing about the war- He did explain their use of “Burn Pits” & how he Stirred them” He still has scars on his hands & feet from “Jungle Rot” I was told by a friend.
Again this really is about Him but I do feel neglected in this whole picture! I also had NO IDEA that “Bad Dream ( Night Terrors) could still happen after so long! It is hard to experience these with him all these years! Yes, he is the one who lives them but I listen to the “Gut Noises” & if it is at all light- or near morning -I see his
“Scared or Mad” face as he thrashes &/or bolts straight up in bed! This is a very kind & gentle man but he still has constant mood problems-I am most often the recipient of his very Verbal anger! I will stick by him-till death- as I promised but if he is gone first- will the military do anything for me?? We were robbed of many “Good Times in our Marriage”. Marriage is never easy but this bad stuff Needs to be blamed on “His Service” we still live this!
Sign me,
53 years as Wife of :
Hal Timothy Mettee
82nd Airborne 1st of the 508th
I have been there for him since 1965- Sorry I had to get this off my chest ! I have paid for private counseling our whole marriage ! He at least has had the VA.
I HAD TO get the rest of this off my chest- Please forward to the proper location! We have been together since 1965!
I STILL WOULD BE WILLING TO HELP ANY VET DO TELE-HEALTH IF NEEDED- that was my ORIGINAL MESSAGE SORRY BUT WE DESERVED A BETTER MARRIAGE- He is a wonderful person!! ?. I hope I will not be forgotten or ignored if something happens to him! Just saying !
I’m a woman veteran and I don’t think 100% is accurate because I could not figure out how to use my cell phone or computer to telehealth my last appointment with my provider.
I need help how to operate a computer I do have one but I need help setting it up to learn more about veterans benefits and health care how do I go about signing up for a program to help me how to use a computer is there a school or the library or someone to come to my home to help or for me to go somewhere to class to learn how to operate A computer need help I was in the United States navy 1970 to 1975
Question: does a “tele- Health” visit cost me the same as a physical visit?
Many older veterans don’t have any devices besides their phones. Without internet services they cannot connect to VA Health.
I would love to get an IPad so I can video connect with my Drs! How can I get
one? Mark Cain
I’ve got poor internet service.
I need an IPad so I can video connect with my Drs. How do I get one¿