At VA, doctors are changing their approach to helping Veterans coping with chronic pain ––an affliction that impacts the lives of at least 100 million Americans.
The Huntington VA medical center in West Virginia, for example, now has 947 fewer patients on opioids. That’s a reduction of 21 percent. The facility also has 753 fewer patients on long-term opioid therapy ––a 23 percent reduction.
An opioid is a drug such as morphine or oxycodone. They ease pain, but they can also cause physical dependency.
“Here at Huntington, as well as other VA facilities across the country, we are offering complementary and alternative therapies for pain control,” said medical center director J. Brian Nimmo. “These alternatives include acupuncture, animal-assisted therapy and art therapy.
“In an effort to expand our acupuncture services, we’re in the process of hiring a psysiatrist who is also trained in acupuncture,” he added. “These and other efforts will continue as we strive to find new and better ways of alleviating the chronic pain being endured by so many of our Veteran patients.”
The same story is unfolding at the Minneapolis VA, which in 2011 launched an effort that has significantly reduced the use of opioids among the Veteran patients under its care, thus improving their chances for a better quality of life.
“Since starting the program, we’ve been able to decrease high-dosage risky opioid use among our patients by nearly 70 percent,” said Dr. Peter Marshall, director of primary care pain management at the Minneapolis VA.
Teamwork Equals Success
“We use a team approach to pain management,” Marshall explained. “Our primary care doctors, pharmacists and mental health professionals all work together to help our patients reduce their long-term dependence on potentially habit-forming drugs.”
Similar strategies are now being used at VA medical centers throughout the country. This nationwide effort, formally known as the Opioid Safety Initiative, was chartered by the Under Secretary for Health in August 2012.
The Opioid Safety Initiative includes key clinical indicators such as the number of individual pharmacy patients dispensed an opioid, individual patients on long-term opioids who receive a urine drug screen, the number of patients receiving an opioid and a benzodiazepine at the same time (which puts them at a higher risk of adverse events) and the average morphine equivalent daily dose of opioids.
 The basis for the Opioid Safety Initiative is to make the totality of opioid use visible at all levels in the organization.
The basis for the Opioid Safety Initiative is to make the totality of opioid use visible at all levels in the organization.
Less is More
Marshall said VA is clearly moving in a new direction when it comes to managing chronic pain.
“We’re moving toward fewer pills, fewer shots and more self-management of non-cancer chronic pain by teaching patients how to change their behaviors, as well as their lifestyles,” he said.
“The whole idea behind our Opioid Safety Initiative,” he added, “is to teach Veterans how to manage their pain in a more effective way ––how to lead a more normal life, even if they have chronic pain that can’t medically be cured.”
Difficult Concept
At the VA medical center in Philadelphia, for example, yoga and cognitive behavioral therapy are employed as part of a comprehensive pain care approach, along with a seven-week course in pain management.
“Convincing someone that we’re going to help them improve the quality of their life, but without making all their pain go away, can be a difficult concept for some of our patients to grasp,” said Nancy Wiedemer, pain management coordinator at the Philadelphia VA.
“We had a young Army veteran here who was in his early 20s when he started on opioids,” she continued. “By the time he came to us he’d already been on opioids for six years, at a fairly high dose. It took a lot of education and support, but we were able to help him taper off. He’s been off opioids for seven months now and he actually feels much better.”
Right Dose, Right Patient, Right Reason
At the Ralph H. Johnson VA Medical Center in Charleston, a little less than three percent of the total patient population is on chronic opioid therapy. That’s five percent below the national percentage for patients receiving such drugs.
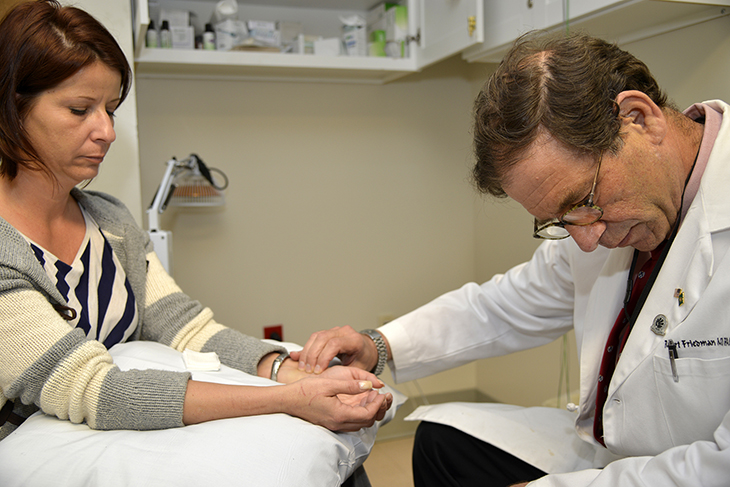
“Opioids have been around for 3,000 years,” said Dr. Robert Friedman, head of the medical center’s pain management team. “They’ve been around that long for a reason. They work. But it’s important that we find the right dose, for the right patient, for the right reason. And that’s what our pain management team here in Charleston does.
“We spend a lot of time learning about the patient,” he continued. “Because the fact is, there are a lot of Veterans who’ve been on opioid therapy for a long time who would do just as well, if not better, without opioids —or on a reduced dosage.”
During the last five years Charleston’s pain management team has helped more than 400 Veterans ease off their pain medications. “A big part of our success,” Friedman observed, “is getting patients involved in their own care, educating them about pain management and supporting them as they try alternative methods for dealing with chronic pain.
“There’s nothing magical about what we’re doing,” he added. “All we’re doing is taking the time to talk with our patients and learn about them.”
It’s All in Your Mindset
There will no doubt be challenges that accompany this new strategy. Patients as well as their health care professionals will need to adopt a different mindset when it comes to dealing with pain.
“This change will require a shift away from simple answers,” warned Dr. Peter Marshall of the Minneapolis VA. “Additional training and support will be needed to build pain management skills for front line primary care teams, and to provide the necessary education to patients regarding the benefits of alternative approaches to managing chronic pain.”
It’s not that opioids aren’t valuable or useful drugs for easing pain, the physician noted.
“Opioids work well in patients who are in acute pain,” Marshall said. “Maybe you’ve been seriously injured, or just had surgery. Maybe you’re dying of cancer. In these instances, opioids are appropriate.
“But when you use them over a long period of time to control chronic pain, it’s a different story,” he continued. “There’s considerable and growing evidence of the harms caused by opioid pain medications, especially at high doses. Your body adjusts to the dose. You need higher and higher doses to get the same relief.”
“Pain,” he added, “is a complex problem that is not solved with a pill.”
Complexities aside, convincing someone to give up their pain meds is likely going to be a hard sell, in many cases.
“This kind of approach takes a lot more engagement from the patient,” Marshall admitted. “We’ll need to monitor them closely. We’ll need constant feedback from them. And they’ll need support. They’ll need to know they have a team around them, helping them on this journey.”
To learn more about pain management at the VA, visit VA’s website.

Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.






EASY FOR U TO SAY.
TRY LIVING ONE DAY WITH MY PAIN.
BEST WAY TO REDUCE BUDGET, TAKE MY PAIN MEDS.
IF I HAD TO GO TWO DAYS WITHOUT THEN, I’D BE YOUR 23rd. SUICIDE THAT SECOND DAY.
MG9M
Nice sounding propaganda piece. No doubt this comment will be deleted like our words and abuse is not heard in Indiana. Why not post how the VA feels “if one veteran on opioid before burns his house down for drug money, then we all will.”
Tell the public that your sites on pain is a lie. Migraines, artificial joints put in wrong, spine/joint pain, nerve pain and etc., is not considered pain issues? That the revolving PCPs at the VA care nothing about patients and few can read the thousands of patients medical records, just concerned about dropping the smallest amounts of pain meds just to appease the medical boards ie. licensing medical boards, teaching colleges and etc. So that the politicians and all medical people have a great part in this fiasco while laughing all the way to the bank with big Pharma?
Why not tell people that YOU “demand” the vets drop pain meds and “forced” to use SSRI and other head dope instead, which creates more issues and problems.
Why don’t you ever listen to complaints when people write to you or email with their concerns about corruption, abuse, racism towards whites, to professional misconduct, or why it’s so difficult to get information on our so-called care givers?
Tell them you want vets to drive hundreds of miles while using their pain meds regardless of DWI laws. OR that we are supposed to take our meds by hourly conditions instead of ‘as needed.’ Or, that no blood test showing lesser use of meds will be considered criminal and also used against the vet.
How about all the foreigners hired at the VA that don’t care about Americans? Who think that since third world countries and people can get by with amputations, etc., get by fine without the likes of American styles care and get by fine?
This is a waste of time trying to talk to anyone from the VA when our Patient Advocates and other phonies have to fear like the vets, retaliation from the VA, deal with threats, flagging, abuses, being totally ignored, countless contradictions in care, and with new pain care clinics told we cannot use civilian care at all. Not with broken bones, heart attacks, migraines etc, we are to drive hundreds of miles to the pain clinic at the VA hospitals. And more ignorant expectations.
What a joke this Draconian system is, socialism compounded with fascism, corporal punishments, complete with Marx-feminist man haters and other idiots there for pay checks and easy employment at some VA centers.
Oh but Congress to the local politicians and city workers get what we can not. Not wasting any more time on this since it will be deleted and those in Indiana and the government or advocate don’t care a bit. They just serve the dictates of the VA and not concerned about us at all.