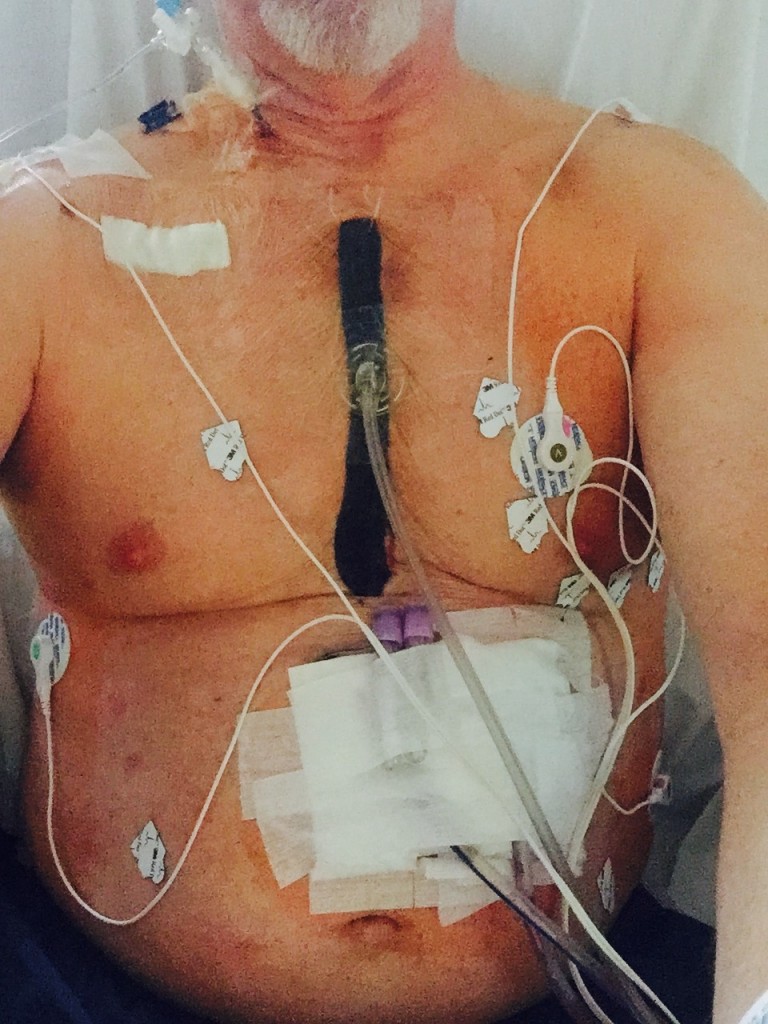
On March 27, 2015, I had open heart surgery for aortic valve replacement (AVR), as well as an ascending aortic aneurysm performed at the Durham Veterans Administration Medical Center (VAMC), which was awesome! I received an artificial valve made of carbon. Before the surgery, I was at risk of my heart getting enlarged and heart failure, all at the age of 54.

On Christmas Eve day, I went to the Durham VAMC for the first time. It was exceptionally quiet, as the President had granted a federal holiday on Dec. 24. I confirmed with the VA that they still wanted me to show up, and I received a warm, “Of course we do. It was already scheduled.” I went to the cardiac area to meet Susan Roberts, LPN. She thoroughly explained what the cardiac catheterization was and the AVR procedure. Then, I talked to the surgeon performing the catheterization. He was very professional and took time to alleviate any reservation I had. I asked him how many times he had performed this procedure and his reply was “over 1,000 times.” This level of experience really made me feel good about being at the VA.
On January 23, 2015, my cardiac catheterization was done to get more accurate readings about my heart, as well as to check for any blockages. When I was wheeled into the OR for the procedure, it was like a NASCAR pit crew was working there. Everything was happening just like it was supposed to. Commands and acknowledgements were called out and confirmed. I was asked if I had ever had this done before. I answered “No. Have you ever done this before?” The reply back to me was “Sir, we do about six of these a day.” That really boosted my confidence in the team. I did not feel anything during the procedure. While in the recovery area, someone I would affectionately refer to as “my PA”, Kista Hurley said everything went great. She then said, literally, “I have good news and bad news. The good news is that you don’t have any blockages or other issues. The bad news is that you will have to get that valve replaced.” It was news I did not want to hear, but did not surprise me.

Dr. Judson Williams performed the AVR and Dr. Jeffery Gaca, from Duke University Hospital performed the aneurysm repair. This procedure was incredible. There were not any complications. Dr. Williams and Dr. Gaca are talented, dedicated, and personable. If you need open heart surgery, see them! Dr. Williams told me that my post-surgery recovery was progressing remarkably. My replacement carbon valve is the very latest technology.
On April 3, 2015, I was discharged! I am blessed to have left the Durham VAMC with a new lease on life. I thank God for placing the doctors, the nurses, and the technology before me to enable a wonderful outcome. I thank my wonderful friends and family for their tremendous support.
As of mid-August, I am 20 weeks post-surgery, and I am recovering wonderfully. I’ve bicycled over 1,200 miles since the surgery and have two week long bicycle adventures on my schedule, each ride with 200 wounded, injured or ill veterans and active duty service members.
About the author: Mike Thomas is a 28-year Veteran of the US Army who receives his health care at the Fayetteville VAMC. He currently serves as an administrative office with the United States Army Forces Command in Fort Bragg, N.C. In his spare time he is an avid cyclist.
Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.