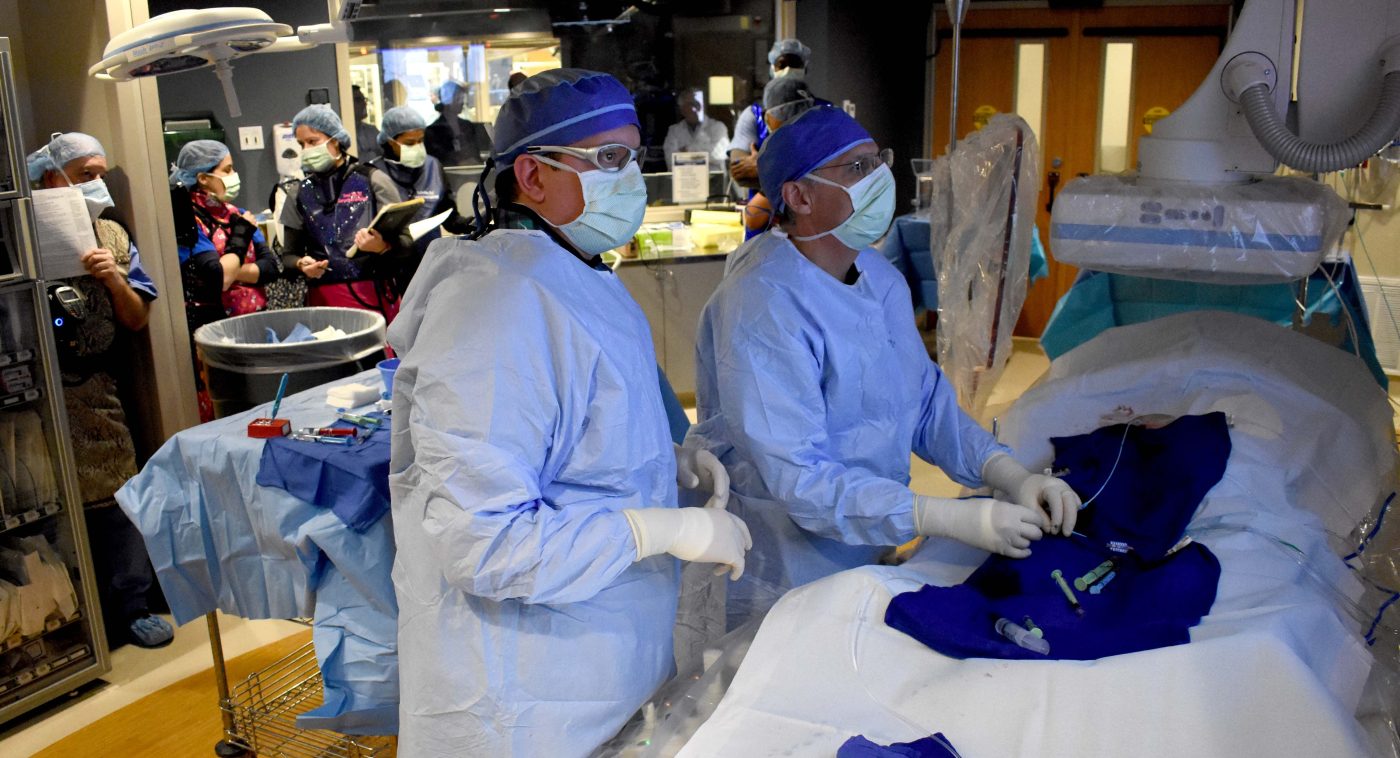
Dr. Jorge Lopez, VA North Texas interventional radiologist, conducts a Y-90 radioembolization procedure on a patient at Dallas VA Medical Center. Y-90 is one of the newest procedures offered at the hospital.
The liver is one of the body’s most important organs. It performs various critical functions to keep the body free of toxins and harmful substances. Unfortunately, some Veterans have Hepatitis C virus, a damaging liver infection, as the result of various exposures during their military service. In addition, these same Veterans are counted among the 42,000 Americans that are diagnosed with liver cancer and related tumors each year because of Hepatitis C.
Thankfully, VA North Texas’ interventional radiology team is giving its affected patients an opportunity to eliminate these tumors with a procedure that can have them home and resting the very same day.
Y-90 Radioembolization is a minimally invasive procedure to treat and eliminate liver tumors without surgery. Tiny glass or resin beads filled with the radioactive isotope Yttrium-90 are placed inside the blood vessels that feed a tumor. This blocks the supply of blood to the cancer cells and delivers a high dose of radiation to the tumor while sparing normal tissue. It can help extend the lives of patients with inoperable tumors and improve their quality of life.
The interventional radiology and nuclear medicine teams work together to make this all possible. Nuclear medicine has a critical role in calculating the correct Y-90 dose for the patient, handling of the isotope, and the overall procedure safety.
“Y-90 is very good at treating the larger tumors and it’s better than anything else available,” said Dr. Jorge Lopez, interventional radiologist at VA North Texas. “Y-90 is an amazing outpatient procedure. The patient goes home that day, compared with surgery, where you may be in the hospital three to five days with a few months of recovery.”
During a pre-screening, the patient gets an ultrasound on their liver and if there is something suspicious, they get an MRI or CAT scan to find the tumor.
“We have many patients with hepatitis C and a certain number of those will develop cirrhosis,” said Dr. Gordon Butler, VA North Texas, an interventional radiologist. “A lot of time tumors are found early because of the screening program, and sometimes there are many tumors, or they are large, so one way to treat those patients is with Y-90.”

Dr. Gordon Butler, VA North Texas interventional radiologist, conducts a Y-90 Radioembolization procedure on a patient at Dallas VA Medical Center. Y-90 is one of the newest procedures offered at the hospital.
The radiation from Y-90 continually decreases over a two-week period and disappears after 30 days. The tiny microspheres remain in the liver without causing any problems.
Y-90 offers VA North Texas patients a minimally-invasive way to prolong their quality of life and get them back to their families, friends and daily routines in a very short amount of time. For VA North Texas interventional radiologists, the procedure offers greater opportunity to blend technology and care.
“The mission of the VA is to repay a promise made to the Veterans by providing exceptional healthcare services,” said Lopez. “This is one of the areas where we deliver that exceptional care.”
Jennifer Roy is a public affairs specialist for VA North Texas Health Care System. She is a retired USN Chief Petty Officer, public affairs manager and award-winning photojournalist.
Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.