While in treatment for aggressive prostate cancer at the VA Puget Sound Health Care System in Seattle, Navy Veteran Allen Petchnick faced a daunting situation. His PSA blood test, the main screening tool for cancer of the prostate, had risen to 13, which for him was dangerously high. Plus, his cancer had spread to other parts of his body.
“He was looking at very tough outcomes,” says Dr. Bruce Montgomery, an oncologist at VA Puget Sound. “He was passing out because his tumor had metastasized to lymph nodes in his neck, which was pressing against one of his arteries.”
Montgomery led a team that performed DNA sequencing on tissue from Petchnick’s lymph nodes. They spotted mismatch repair (MMR) deficient cells, which usually have genetic mutations that could lead to cancer.
Petchnick received immunotherapy, a form of precision oncology in which organisms in the body’s immune system are used to fight cancer. Now age 79, he’s been on immunotherapy drugs for nearly two years. His PSA level has become undetectable and the tumor continues to shrink, Montgomery notes.
“He went from basically being unable to get out of a chair to going shopping with his granddaughter in just one cycle of therapy,” Montgomery says. “He may be cured. But we’ll only know that when we stop his therapy, which is likely to happen soon. Right now, he’s very close to a complete response after looking like he was going to be in very difficult straits.”
“He went from basically being unable to get out of a chair to going shopping with his granddaughter in just one cycle of therapy.”
Petchnick is one of several success stories arising from a partnership between VA and the Prostate Cancer Foundation (PCF), a philanthropic group that funds research to prevent and cure prostate cancer. The partnership is speeding the development of treatment and cures for Veterans with aggressive—or metastatic—prostate cancer through precision oncology.
The process involves the molecular profiling of tumors to identify genetic mutations that can be targeted through means such as immunotherapy or chemotherapy. Targeted therapy attacks the genes, proteins, or other biological elements that are specific to a tumor and make it grow.
VA and PCF signed the agreement in 2016 and put it into action early this year. It comes at a time when more than 16,000 Veterans are diagnosed each year with prostate cancer, making it the most common solid tumor cancer among Veterans.
Rebecca Levine, national director of PCF’s Veteran health initiative, says the foundation felt compelled to partner with VA also because some of its board members are Veterans who had life-extending results after participating in prostate cancer trials. “Those patient stories made it very clear to us in a personal way why this is so urgent and how transformational the opportunity to partner with VA can be,” she says, “given what PCF brings to the table in science and what VA brings to the table with its large patient population.”
In Bruce Montgomery’s view, PCF decided that investing its research dollars in a national integrated health care system like VA would provide the most impactful return.
“There was obvious interest on their part in precision oncology,” he says. “They also saw VA’s resources with regard to integrated data and clinical elements as something that could in the big picture and over the long term provide critical insights into how we might reach men who have advanced prostate cancer and give them the best access to health care.
“The whole idea behind this effort was to stand up an integrated precision oncology system in VA and show that if we can do this in the biggest health care system in the U.S., then the optimal efficiency and outcomes can be extended outside of VA and provide better results for everybody.”
Currently, nearly 500,000 living Veterans have been diagnosed with prostate cancer. Of those, an estimated 3% have metastatic prostate cancer.
PCF donated $50 million to VA in the five-year partnership. It calls for increasing the number of VA facilities that are doing precision oncology and prostate cancer clinical trials, raising the number of VA researchers applying to PCF for funding, and getting more Veterans enrolled in studies. About half of the funding is aimed at building a network of VA sites that are doing precision oncology. The network now includes 10 sites: Washington; Philadelphia; Seattle; Los Angeles; Ann Arbor, Michigan; Durham, North Carolina; Tampa, Florida; Bay Pines, Florida; and New York City, in Manhattan and the Bronx. The goal is to eventually have at least one network site in each of the 21 VISNs (Veteran Integrated Services Networks) into which the VA health care system is divided.
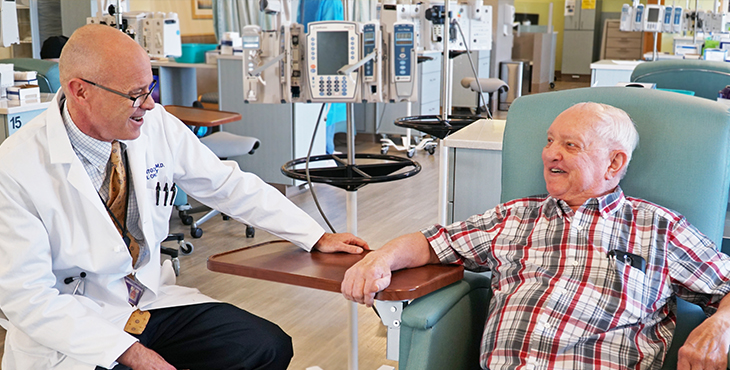
Photo at top: Dr. Bruce Montgomery meets with Navy Veteran Allen Petchnick, whose prostate cancer has been effectively treated to date with targeted therapy. (Photo by Christopher Pacheco)
To read a longer version of this story, visit the VA Research website.
Topics in this story
More Stories
Diverse representation of women in health care research allows MVP to make discoveries for women’s health
Join the Million Veteran Program online. You will have the option to receive an at-home blood sample collection kit in the mail.
VHA's new podcast series, New Horizons in Health, features a candid discussion of psychedelic assisted therapies for Veterans experiencing mental health conditions.






Like to hear from you
What to do after your prostate is removed?what plan of action can you do to get back to normal?
I am taking finasteride for Bpi for years now and wondering if psa test will present false readings . I’m worried cause I’m having problem urinating with pain . No semen comes out upon ejaculation plus painful eject. I am 78 yrs old. Urinate dribbling all day and my urge seems to be every 15 minutes. Also wake me up at night to urinate. Can you help me?
It’s no walk in the park, but having a loving caring family behind you will make it much easier. I had the robotic surgery done at Stamford by the best Doctor and staff on the planet. My son was there to drive me whenever it was necessary, and last but certainly not least was a loving caring wonderful wife that was there every step of the way. NOW, prior to discovering I had prostrate cancer, my first Urologist told me I needed testosterone injections because my T score or something like that was low. He told me it would help with my sex life etc. Well I learned after the surgery that cancer feeds on the injections and it almost killed me.My wife begged me not to take the injections saying that was the last thing I needed and she was correct.
After the surgery my PSA score was still readable and a Doctor advised me to undergo radiation to ensure eradication of any remaining cancer. Well, I underwent the radiation process and the doctor assured me the cancer was indeed completely gone.However, ah yes the however word, it would leave me impotent and incontinent which it did. I have been able to work around the incontinent which requires me to get up to go pee every couple of hours, as long as I don’t drink coffee.and I wear a small folded towel in my underwear for minor dribbles. It’s been nine years now and still completely without cancer. Many thanks for the doctor at the VA for discovering my cancer. And for the doctor that caused my cancer to go sky high from the injections, “No comment” he is now retired. PS, I am now 81 years old and living well due to a wonderful wife.
Joe,
I am thinking of going with the proton therapy for my prostate cancer. How many treatments did you have? No side effects ???
Thanks,
Andy
I was treated for Prostate CA in 2009 using Proton Beam therapy. Treatment took 44 treatments, one a day Mon. through Friday. (approx 9 weeks) My current PSA is under 1.0 and bi-annual PSA test have been discontinued. I have had virtually NO side effects. There is a book I would recommend: “You Can Beat Prostate Cancer and you don’t need surgery to do it” by Robert J. Marckini.
I am 73 and my VA doctor will not authorize a PSA test. She says nobody over 70 dies of prostate cancer. Now when I need to urinate I can’t get beyond 10 feet without leaking into my boxer briefs. I am taking a prescription that takes 6 months to work. What else can I do but go to a private urologist?
Gary, it sounds to me like you might need to find another doctor, or at least get a second opinion under Medicare, seeing as how you are age-qualified for Medicare. The PSA test takes all of a few minutes and consists of a simple blood draw, and that specimen is then sent to a lab for analysis. It is very routine, especially during the annual physical exam, and is generally covered under Medicare. It seems inconceivable to me that the VA doctor will not approve such a simple and relatively inexpensive diagnostic lab test. I believe she is also probably very wrong in her theory that “nobody over 70 dies of prostate cancer.” While it is, in many cases, a very slow growing form of cancer, it can be very aggressive, and, left untreated, many seniors have been known to have it at death, but might have had a different disease “officially” declared as their cause of death, rather than their prostate cancer. But, prostate cancer does kill, and it isn’t always the elderly! My prostate cancer was caught at a treatable stage, due to PSA tests and a needle biopsy, and I’m very fortunate. If you have Medicare, you should find another doctor and have the PSA test done, even if you have to pay a modest co-pay out of pocket. Just my humble opinion as a (Stage 3) prostate cancer survivor. By the way, in addition to Medicare, as a retired federal employee, I’m fortunate enough to have an affordable GEHB Blue Cross Blue Shield secondary policy, so between Medicare, as the primary payer, and BCBS, as secondary payer, I have yet to pay a co-pay for anything since I went under Medicare over five years ago.
You are seeing absolutely the worst possible doctor on the planet. You need to go over her head to the administrator of the hospital, or VA Med center and present this to that person. She needs to be fired immediately for this malpractice and I would also contact a lawyer to get advice on suing her for the malpractice. I’m very serious about this. My cancer was diagnosed when I was 73 and had the robotic surgery for removal. Not the greatest outcome of after effects but at least I’m 2 1/2 years down the road and cancer free. I hope you take this advice, at least about talking to a higher up. My best to you and prayers for a successful treatment.
“Bravo Sierra” … heard the same thing … called my congresswoman…. had test found prostate cancer …
Gary, find out what your PSA is! Especially if you are having urinary issues and taking a prescription. My 74-year-old loved one just finished chemotherapy for stage 4 prostate cancer. (No cure, but fingers crossed for extending his life.) It will haunt me forever that I never thought to ask about his PSA because it always was checked during annual physical. Until he turned 70.
When is the VA going to start paying for PROTON THERAPY for prostate cancer?
I am a prostate cancer survivor because of prostate cancer!
Never had a day, or for that matter a minute, of side effects during the Proton Therapy or since.
The VA could save money by going this route as compared to other forms of prostate cancer therapy.
When you are done with the treatment, you are done.
Also Medicare and most private insurance will pay for this.
Go to the Loma Linda Proton Center web site for all you would ever want to know about Proton Therapy.
Or you can contact me and I will be glad to fill you in.
joe i have recently found out i have gleason score 7 (3+4) group 2 cancer. when you said “side effects” were you talking ed, nerve damage,or incontinence