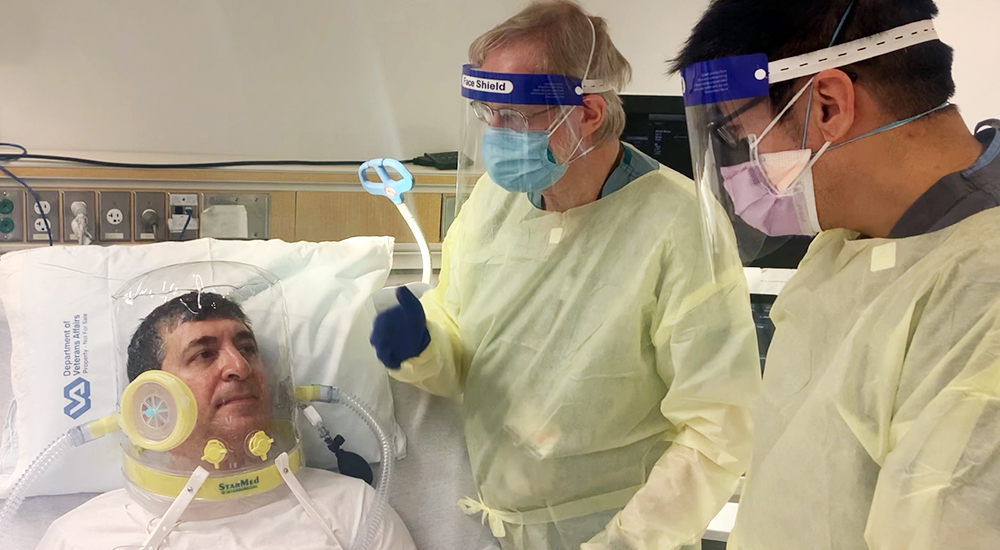
It may look like something from a science fiction movie, but the spacesuit-like respiratory helmets at Chicago’s Edward Hines, Jr. VA Hospital represent the cutting edge in COVID-19 treatment.
Developed in Italy during the early 1990s, respiratory helmets, often nicknamed bubble helmets, are used in hospitals across southern Europe for patients suffering from respiratory distress but are uncommon in North America.
When COVID-19 spread to the United States in March 2020, Hines VA Hospital immediately began looking for ways to treat the mostly unknown virus.
“We were overwhelmed with patients in respiratory distress and we were trying to find a solution,” said Dr. Franco Laghi, pulmonologist at Hines VA.
According to Laghi, the pulmonology team was familiar with early respiratory helmet research and its use during Italy’s first wave of coronavirus. Despite a surge in global demand, Hines VA was soon able to secure the strange looking but effective device.
“It’s been around prior to COVID but it’s really been used a lot during the COVID pandemic,” added fellow pulmonologist Dr. Rishi Mehta. “The basic idea behind it is that you are giving pressurized oxygen to a patient in an interface that is hopefully more comfortable and allows the patient to breathe more naturally.”
According to Laghi and Mehta, the helmet (pictured above) is not for every patient but can offer advantages when used.
Keeps medical staff away from patients’ airways
Helmet treatments can reduce intubations which have high mortality rates. It can be used without mechanical breathing machines in some cases and doesn’t cause skin deterioration from long-term oxygen mask use. Additionally, the bubble keeps medical staff away from infectious patients’ airways by eliminating the need to readjust masks.
Respiratory helmets can also benefit Veterans who have PTSD by not restricting the face, like standard oxygen masks, which can be upsetting, the doctors noted.
Still, its unusual appearance may leave some Veterans initially confused.
“It can look very strange at first for a patient. You see people bringing this big helmet but they adjust very quickly,” admits Edita Vines, respiratory therapist at Hines VA. “They can talk, get a sip of water and they can communicate and see what is going on around them more comfortably in the helmet.”
When the team received their first helmet a year ago, learning how to use it wasn’t easy, Vines noted.
“We used it on ourselves to learn.”
“The training was really limited. We had to find the studies and find the research ourselves,” Vines said. “We started networking with other respiratory therapists and just trying it on, using it on ourselves to learn.”
“The nurses and respiratory therapist took the time to learn it right before we started deploying it on patients,” Mehta said. “They learned on the fly. This is a whole new technology that no one is used to. Usually, this process takes a long time but with the pandemic, they did it astonishingly fast.”
In the summer of 2020, the team was ready to use its tested helmet on a volunteer Veteran in respiratory distress from COVID-19.
“His oxygen levels improved immediately and the patient felt comfortable inside the helmet,” Vines said. “He learned how to manage the helmet by opening the access port to drink some water, take medicine and inflate and deflate the comfort pillow around his neck.”
Procured additional helmets last winter
Since then, Hines VA has successfully deployed the new treatment on other COVID-19 patients. The hospital procured additional helmets last winter.
Hines is among the first hospitals in the nation to use the technology. Vines noted that numerous VA medical facilities have reached out to learn from her team’s experience. Many have purchased respiratory helmets to use at their hospitals.
“We are ultimately here to help the patient,” said Vines. “Since the start of the pandemic, we all ask, ‘What else can you do? What did you learn? Did you know something new?’ We share whatever we do to help others.”
To learn more about VA’s ongoing response to COVID-19 and vaccine rollout, visit www.va.gov/health-care/covid-19-vaccine and facebook.com/HinesVAHospital.
Matthew Moeller is a public affairs specialist at the Hines VA Hospital.
Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.