Staging is critical for pinpointing the best way to treat cancer. In staging, doctors determine where the cancer is in the body so they can address it accordingly, whether through surgery, radiation, chemotherapy or other means.
At the Harry S. Truman Memorial Veterans’ Hospital in Missouri, researchers are testing a new tracer drug for its ability to show whether and where prostate cancer has spread in the body.
Dr. Thomas Dresser, a nuclear medicine physician, and Dr. Timothy Hoffman, a radiopharmaceutical chemist, are carrying out a phase 3 clinical trial on the drug, which contains a pharmaceutical component and a radionuclide component. In the procedure, a prostate tracer drug in a vial is connected to a generator and combines with gallium 68, which emits radioactivity in the form of a positron. That formula, known as Ga68-PSMA-11, is then injected into a patient and binds to the prostate cancer cell because of a protein in the cancer cells called PSMA – prostate specific membrane antigen.
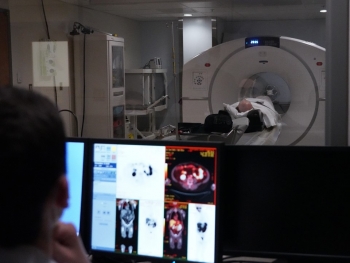
A Veteran undergoes positron emission tomography scanning in the clinical trial. (Photo by Mindy Roettgen)
Procedure more accurate than CT Scan, bone scan
Images from a positron emission tomography (PET) scanner show the location of the cancer.
This type of drug appears to be the best diagnostic tool for staging prostate cancer and determining whether it has metastasized, says Dresser, the chief of nuclear medicine at the Truman VA.
“Once administered intravenously, radiopharmaceutical peptides are attracted to and bind to cancerous cells,” he explains. “When used with PET imaging, these radioactive peptides light up on the scan to identify even the smallest amount of disease in its initial growth. We scan the entire body and can identify prostate cancer with a higher degree of accuracy than a CT scan or a bone scan.
“When a normal cell in the prostate gland becomes cancerous, the membrane of the cell begins to make too many copies of PSMA,” he adds. “This unique cell marker can help us diagnose prostate cancer. However, current imaging does not clearly identify if and where metastasis has occurred. The key to diagnostic precision is the use of this injectable radiopharmaceutical peptide designed for a specific cancer and used in conjunction with PET imaging.”
It’s a game changer
To date, Dresser and his staff have staged cancer in 25 Veterans at the Truman VA who were diagnosed with prostate cancer through biopsies. The researchers are comparing the findings of PET imaging with those of a CT scan and a bone scan. Many patients in the group of 25 have shown upstaging, which is the effect of finding more disease in this case beyond the prostate and changing the stage, according to Dresser.
“This is important because if someone is treated for limited disease when extensive disease is present, they will not receive the cure that was planned,” Dresser says. “They may return in one year and find the disease has returned when, in fact, it was there from the beginning. It may have spread to the lymph nodes, bones and other tissue. But the older methods did not detect it. Historically, we’ve not had a good way to determine where it’s spread. PSMA imaging will greatly improve the management of prostate cancer. It’s a game changer.”
Dresser expects to conduct PSMA imaging on about 100 patients over a year.
More Information
Click here to read the full story.
Click here to learn more about VA research.
Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.







What a bizarre world where conspiracy delusionals such as Susie Queen believe that scientists and doctors spend each day solely focused on new ways to kill people. She and millions of others are still drinking the Rev. Jim Jones Kool-Aid. How pathetic. In contrast I applaud this breakthrough and hope it helps many, many veterans.
wondering if this procedure testing is being passed out to all VA facilities for possible participation/testing????
Can I get into the clinical trail at the James H. Quillen VAMC?
Sounds exciting and useful.
‘1 in 8 old men get prostate cancer’ it says. I had thought it was more.
I’m having increasing problems with incontinence and related problems, so my primary MD will hear about it. Thanks for printing both ling and short versions. Goes to my bookmarks.
Susie, Susie, Susie. Where did you find evidence that anything in the story “kills people”? (Besides prostate cancer.
Which doesn’t kill women.
Boys and girls are different.
Ask your Mommy.)
Research the topic of background radiation, please. That will scare you.
Radiation injected into people that the body can never eliminate…. how freaking game changing! Just inventing new ways to kill people.
Keep me posted. I am schduled for prostate biopsy in early m March 2022. I have illostrmotam for 52 years.and oI am hesitant for a normal biopsy
Loma Linda
[Editor: Do NOT publish your sensitive information on the internet. I have removed it from this comment.]