Every day, clinical teams face situations during the hospital discharge process that require insight and empathy to meet the patient’s needs. These skills are typically developed through experience. But imagine the possibility of offering employee development and education programs that build resilience and enhance empathy and soft skills.
At VA, the Veteran Experience Office (VEO) is collaborating with the Office of Healthcare Innovation and Learning (OHIL) and the VHA Extended Reality (XR) Network to explore a new role for Virtual Reality (VR) in employee education. The collaboration developed a new VR Inpatient discharge application that builds empathy for Veteran patients and provides guidance on effective communication during the discharge process.
A hospital stay can be a confusing and frightening experience for some patients. VR technology can help clinical staff better understand the perspectives of patients and their journeys to discharge, and it can provide a window into the patient’s experience. This new technology can help staff members not only improve communication but gain empathy and navigate difficult conversations by understanding the moments that matter most to Veterans, families and caregivers.
“I think this new training app will be very beneficial, especially now,” said Amanda Rose, VR champion, RN, Orlando VA Medical Center. “Since the beginning of the pandemic, it has been a more difficult time in health care… Employees are experiencing compassion fatigue and burnout with resources, especially staffing, stretched thin.”
 Goal of the training is to build empathy, compassion
Goal of the training is to build empathy, compassion
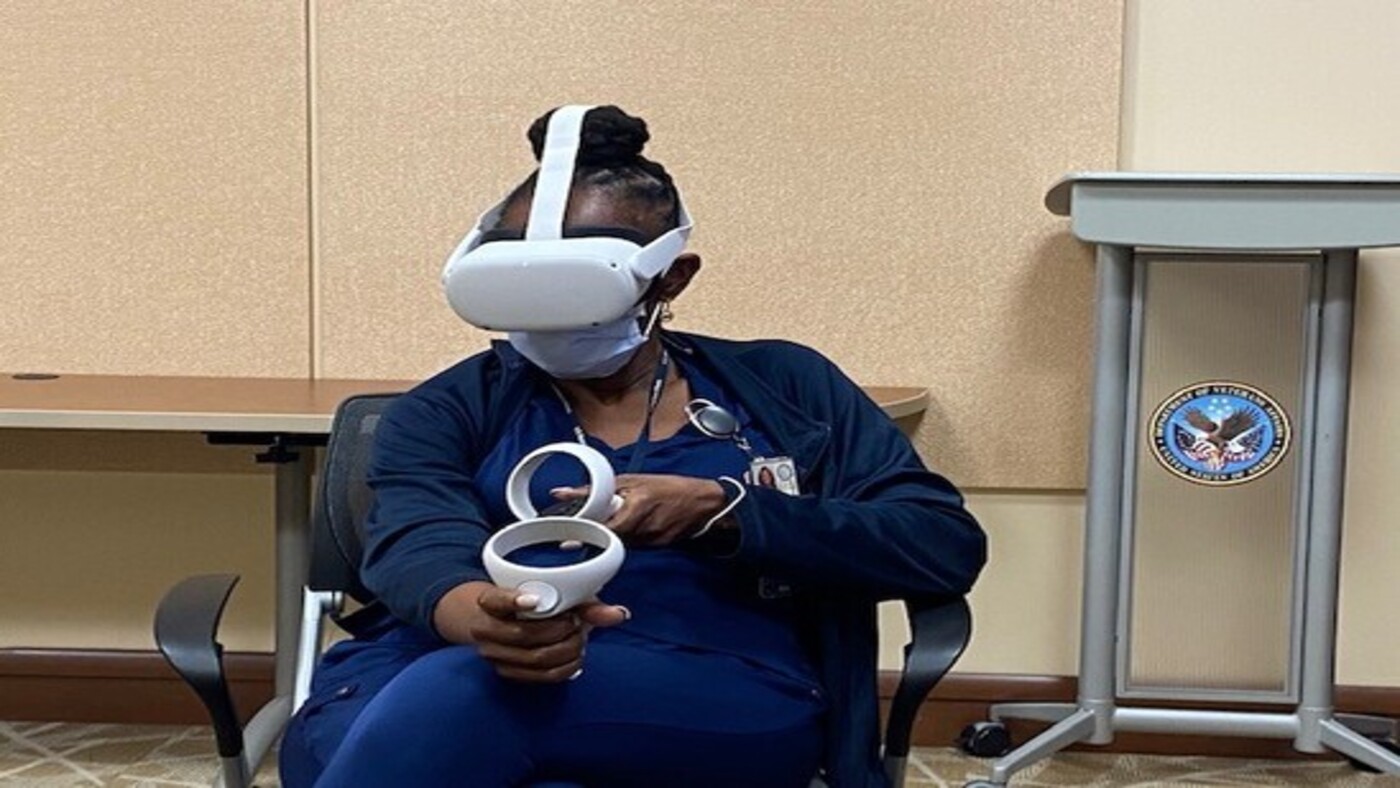
The VR Inpatient Discharge app allows staff to simulate being a patient in an inpatient bed and experience real-life scenarios from a first-person perspective. It aims to empower all VA staff to experience the emotional ups and downs of a Veteran patient navigating through the discharge journey.
Participants are immersed in a realistic virtual world that gives them insight into what it is like to be the patient in bed. Participants can experience the use of the call button, text family members, reach for the water pitcher or food, review the discharge checklist, and experience symptoms and confusion common to inpatients. This allows clinicians and nurses to better understand the patient’s perspective concerning their discharge and to help them prepare for a safe and effective transition from a VA medical center to home or another care environment. The overall goal is to build empathy, compassion and resilience in the hospital environment.
Enhancing discharge procedures to improve patient outcomes
The VR Inpatient Discharge app was recently tested at the Orlando VA Medical Center, where 13 VA employees and one Veteran patient participated in the empathy-building training. The goal was to understand the participant’s overall experience using the VR application and assess its usability.
Sessions lasted 60 minutes and were attended by one participant, facilitator, data logger, VEO patient experience and OHIL/VHA XR Network stakeholders. Each participant spent approximately 15 to 20 minutes in the VR headset. While using the application, participants experienced different scenarios and answered questions describing their overall experience with the VR Inpatient Discharge application. Participants noted feeling empathy for the Veteran patient and validated the day of discharge events after completing the scenarios. Many participants said the discharge experience through the application was insightful.
“It was a good and interesting experience,” said Rose. “You can see things in a different way. It gives you the perspective of what is important to the Veteran and makes you notice things you don’t normally think about.”
Air Force Veteran Robert “Bob” Horner: “I thought it was really cool to see that VA is using these newer technologies and looking for new ways to assist the process of discharging patients from the hospital.”
`This is going to be revolutionary’
VA is focusing more on improving patient experiences. Tools such as the VR Inpatient Discharge app can help to improve patient satisfaction by streamlining discharge procedures and enhancing communication between clinical staff members, resulting in better patient outcomes.
“The overall process is innovative and gives me a different perspective of how the Veteran perceives our care,” said Genevieve Lubin, RN Patient Safety simulation coordinator, Orlando VA Medical Center. “You think that you are providing a certain type of care, but when the tables have turned, and you become the Veteran, you can sense what they are going through.”
As better education results in better health care outcomes for Veterans, VA is trying to radically revolutionize Veteran care and employee experience by testing this new VR application. This new VR technology can help clinical staff empathize with patients on a deeper level by experiencing the journey to discharge as they do.
“I think this is going to be revolutionary, and I believe that this is what is needed to periodically remind our clinicians on Veteran-centric care,” said Lubin. “When I am immersed in this simulation, I get to feel what the Veteran is feeling.”
The VR Inpatient Discharge application will be tested further to gain better insight into patients’ thoughts and emotions in order to improve inpatient discharges at VA. As a result, clinical staff will be able to relate better to the needs of patients and provide more personalized medical services.
“I think it shows the VA’s commitment to go to any length to improve the patient experience,” said Horner.
For questions or to learn more about VA’s use of VR, email VHAXRnetwork@va.gov.
Topics in this story
More Stories
Each week, we receive job announcements from employers and employment websites—including RallyPoint, RecruitMilitary, VetJobs and HireMilitary—looking to hire Veterans. This post contains links to job listings for the week of July 22, 2024. Each week, we’ll continue to post relevant and timely listings as we receive them, and for the locations listed.
VA hosted its second virtual regional Veterans Experience Action Center (VEAC) June 11-13 as part of a series targeting recently separated Veterans and military members nearing transition out of the armed services.
VA Secretary Denis McDonough spoke to Veteran gamers at the Warrior GMR Mental Health and Gaming Summit July 12 in Washington, D.C.





Probably a waste of money!!
Better to spend it on patient care.