“I had the ladder all set up in the garage,” the Veteran said. After years of suffering with serious mental illness and the effects of military sexual trauma, she had decided to end her life. “I had the rope. I climbed up the ladder and looped the rope over the beam. Then my golden retriever came and laid down under the ladder.” Her voice broke. “I just couldn’t do it in front of her.” So the Veteran climbed down off the ladder, put the rope away, and continued to live.
Her story is not unique. Most people who work with Veterans have heard them talk about the importance of their attachment to their pets, and many of us have had Veterans identify their connection to their pet as their primary reason for living. And which of us is surprised? Many of us, Veteran and non-Veteran alike find that our connection to our animals makes our lives richer.
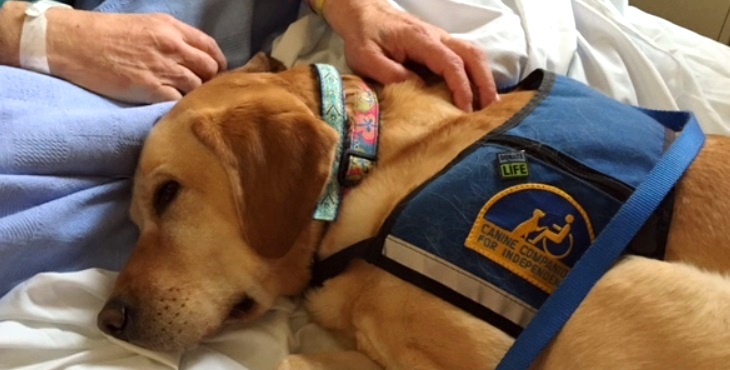
It turns out that the power of the human-animal bond changes lives in the VA medical center as well. In February 2013, our staff at the Denver VA grew by one as I was matched with our new facility dog Waffle, a Labrador Golden Retriever cross. Trained and provided by Canine Companions for Independence, Waffle works with me in my role as psychologist on the palliative care team. Together we care for Veterans who have serious illnesses and those who are at the end of life.
As the palliative care psychologist, I need to connect quickly with my patients in order to gather information, provide support, assess mood and coping, help clarify values, manage pain and facilitate family discussions. Sometimes all of these literally have to unfold in the first contact, and often I have only a few opportunities to connect with Veterans and their families if they are to benefit from our services.
Many Veterans we see in palliative care are in pain, frightened and sometimes suspicious of the VA system and the people in it. Veterans also sometimes express a distrust of psychology, with comments such as “Uh oh, they sent the shrink” or “I’m not crazy!” when I introduce myself. A non-Veteran I once met could have been speaking for many of our patients when he said, “Oh, you’re a psychologist! Are you going to ask me tricky questions and get me to tell you things I don’t want to?”
Working with Waffle has helped open the doors to establishing trust and rapport more quickly, allowing me to more effectively serve our Veterans. This is consistent with studies that show that use of animals in a therapeutic setting can help to make the situation less threatening and assist in healing. For many Veterans, particularly those with PTSD, it is easier to connect with a dog than with humans. Animals don’t care about a person’s material possessions, health and socio-economic status, and social skills, which helps both Veterans and staff find her gentle presence and eager acceptance so comforting.
Palliative care is, by definition, about the relief of suffering. When we introduce ourselves to our patients we explain that “palliative” comes from a Latin word that means comfort, and we call ourselves “Team Comfort.” Our patients are often suffering from a variety of troubling symptoms such as pain, nausea and breathlessness. They also are at what can be a very distressing time in their lives, from a new cancer diagnosis, to an exacerbation of a chronic illness, to the days and hours before death. Frequently, they are grappling with existential issues as well as depression and anxiety. Some also have a history of serious and persistent mental illness. Waffle loves them all, and for most of them she brings a smile and a moment of comfort in a world that is otherwise distressing and painful. Her comforting presence is also a gift to Veterans’ families who are struggling with the burdens of caregiving, difficult decisions about end-of-life care, family conflict, sadness about the losses of the veteran and family, and the grief of bereavement.
We recently completed a study, in collaboration with Dr. Cheryl Krause-Parello on the nursing faculty at the University of Colorado School of Medicine, that found that Veterans’ heart rate and cortisol (a biomarker of stress) dropped after a visit with me alone, but dropped more significantly when Waffle and I visited them together. So we have biomedical data in a controlled study to show us what our hearts already knew – that the presence of a loving animal can make humans’ hard times easier.
I saw this in action recently with a Veteran who had an incurable infection in his pelvic bone. His only choices were undergoing a huge surgery that would remove half his pelvis (and the attached leg), reroute his bowel and bladder system, and entail weeks on intensive rehab – or not undergoing the surgery and living the best quality of life possible until he dies of the infection. He came to a meeting with more than a dozen providers from medicine, palliative care, infectious disease, general surgery, orthopedic surgery and nursing. With no family or friends, he sat alone facing this circle of strangers and facing this tremendous decision. He was struggling, shouting, understandably frustrated and afraid. Waffle quietly got up from her place at my side and lay down in front of him. It struck me at that moment that he had been so very alone, but with that one gesture Waffle made it so that he had an ally.
As with the Veteran on the ladder, as with so many of our Veterans, and as with so many of us who care for Veterans, our animals can be our friends and sometimes our lifelines.

Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.






Dr. Holman’s vita prior to psychology gives a peek at her soul–a mindful soul.
Caring is the essence of the treatment we suffering vets need.
where do we take our dogs to train them to be our campanion
How do you get a dog ? I am a vetrean 100% disability!
Wow, would love to meet WAFFLES!
I WOULD!
Having been a PTSD victim I can assure you that companion dogs help Vets at home. Companion animals do not judge you and let you talj and give unconditional love. The VA needs to work with shelters to encourage adoptions for Veterans.