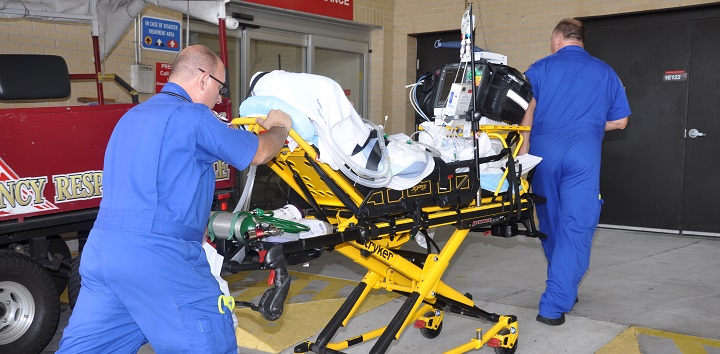
VA’s Veterans Health Administration (VHA) is responsible for providing timely access to Veterans for acute inpatient services across the country. This capability is especially important during natural disasters—such as hurricanes—so that Veterans may be transferred safely to alternative care locations. During the 2017 hurricane season, with three major hurricanes hitting the United States and U.S. territories, VHA’s bed management capability was tested. This test confirmed VHA’s Bed Management Solutions (BMS) program as a critical tool for emergency management.
Managing patient flow during a natural disaster requires hospital staff to be able to view available beds at any of VHA’s 144 medical centers across the nation, and is critical in identifying Veterans waiting for beds including their required specialty. BMS provides this system-wide view to facility staff while also providing emergency management icons to identify specific patient requirements, such as wheelchair transport, electric wheelchairs, stretchers, lift equipment, negative pressure, oxygen, ventilators, one-to-one or service animals. Emergency reports are also available to assist leadership with evacuation decisions or post-event follow-up.
Charles Tupper, assistant director for emergency management at the Charleston, South Carolina, VA, explained, “On a day-to-day basis, BMS allows the emergency manager to quickly look at the status of the facility in the same way that a pilot looks at a manifest prior to take-off. You need to know how many ‘souls on board’ you have in case of some off-the-wall catastrophic event like a fire, terrorist event, or natural disaster. For a more structured or ‘planned emergency,’ like an impending hurricane, BMS gives you the opportunity to quickly identify the patients and residents needing movement, what equipment and supplies they will need, then tag them, roster them, manifest them and get them out the door. BMS is an evolving and ever-improving product and I feel that emergency management will always need to play a part in the fine-tuning and improvement of the product.”
VA’s regional health network, VISN 16, which includes the Houston metropolitan area, was severely impacted by its direct hit from Hurricane Harvey, as well as indirectly affected by facility disruptions due to Hurricane Irma six weeks later. According to Stephanie Seaton, utilization manager and flow coordinator for VISN 16, hospital staff accessed BMS software daily to identify potential needs and the capacity available at other VA facilities. “The software’s transparency and availability of information allowed for prompt and efficient responses to our emergency operations center, helping to coordinate care across the network and the country pre- and post-BMS implementation. This tool adds so much value in inter- and intra-facility flow management not only at the facility level, but also the VISN and nationally,” Seaton said.
In San Juan, Puerto Rico, BMS has assisted hospital staff in the VA Caribbean Healthcare System with coordinating patient flow and managing overcrowding within the emergency department. In San Juan, there were days without hope of having enough beds for patients in the emergency department since Hurricane Irma made landfall. Additional patients were brought in by San Juan’s Emergency Management System, seeking humanitarian assistance and medical care due to injuries post-hurricane. This required many patients to wait a week for a specialized bed while their care was managed in the emergency department. Community hospitals were experiencing similar delays, so when a Veteran approached a community facility searching for care, the request for transfer to the VA hospital was automatic using BMS. “Thanks to having the Bed Management Solution program, we were able to manage discharges and admissions and use the admission order time available through the software to assign available beds in an orderly fashion,” Emilio Hernandez with VA Caribbean Health Care System explained.
Hernandez also said that BMS helped bed management staff to demonstrate to leadership the need for setting up a shelter in the facility to move discharged patients—and provide beds to those seeking humanitarian assistance, but not requiring medical care—so that patient flow could be maintained. “As of now, we have not had the need to evacuate the facility or to transfer patients to other VA facilities across the nation, and our medical center has been able to manage our continued critical flow situation. With the use of BMS as our flow tool, we are caring for our Veterans the way they deserve.”
VHA and the Office of Systems Redesign and Improvement are committed to the development and enterprise-wide use of BMS as its primary bed/patient tracking system.

Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.