Surgeons at the VA Medical Center in Washington, D.C., have begun using a new class of biological resilient tissue valve. It’s believed to be a dramatic improvement over traditional bioprosthetic (tissue) valves and mechanical valves for certain patients.
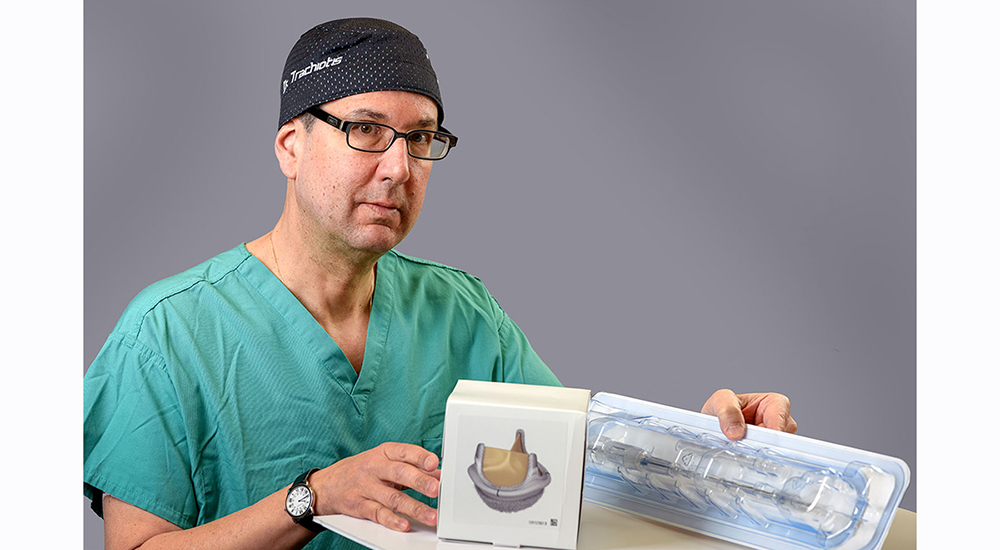
Dr. Gregory Trachiotis is pictured above with one of two new surgical valves: the sutureless (Intuity) valve that can have advantages in Veterans who are older, need other complex cardiac procedures and potentially shorter operative times for aortic valve stenosis.
The only medication needed is a baby aspirin taken daily.
Trachiotis is chief, Cardiothoracic Surgery and director of the Heart Center at the DC VA medical center.
The other valve, Inspiris, can be suited for the more active and younger Veteran with aortic valve diseases. The DC VAMC was the first VA in the country to implant these valves.
The new class of biological resilient tissue valve is for patients with heart failure and those suffering from fatigue or shortness of breath with exercise and who have passed out because the aortic valve is tight. Prior to treatment, the proper decision for any valve replacement therapy is always discussed with a heart valve team.
The new design treatment option has a preservation process that enhances the longevity and durability of the valve. It’s especially promising for youthful energetic Veterans with aortic valve disorders. The current engineered bioprosthetic valve in a 50-60-year-old may last 20 years.
Valve is longer lasting and resists calcium buildup
Trachiotis: “The new class of resilient valve is especially beneficial to our younger patients who want to maintain an active lifestyle.”
The new biological valve is longer lasting and resists calcium build-up, eliminating the need for blood thinners. For the younger patient, if the valve fails as they age, it is uniquely designed to facilitate a trans-catheter valve in valve (TAVR) procedure, reducing the likelihood of a major cardiac operation. The only medication needed is a baby aspirin taken daily.
Younger patients with the alternative mechanical valve are required to take blood-thinning medication for life to prevent thrombus or clot formation. Mechanical valves also are not suited for a (TAVR) procedure should the valves ever fail.
Over 25 successful Veteran surgeries so far
The new therapy has been used in more than 25 patients so far with excellent results. The DC VA is the first VA in the nation to use the valve and is an early adopter of a suture-less valve which reduces operation time. It also facilitates small incision surgery and is good for patients requiring other cardiac procedures at the same time
Employing the latest advancements in heart valve replacements demonstrates VA’s commitment to continued innovation and providing the best possible care for Veterans.

Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.






My dad is a veteran and has aortic stenosis. What is the procedure for evaluating if he is a candidate for this procedure? His local heart doctors do not seem to be doing anything to relieve his difficulty with breathing and shortness of breath. It’s very concerning to me they can not do more than they’re doing. His heart value issue started a few years back. The doctors tried a procedure where they went in through the artery and placed a stent to help the heart muscle work better and provide more oxygen in his blood. This however is not working the way is should anymore. It’s hard for me it see him in this condition. His limited movement around the house and limited duration of just walking from point A to point B. He sounds so out of breath every time we speak to him over the telephone. Is there nothing anyone can do? He was so active a few years ago. Now he can hardly breath. I’m will to drive to Washington DC from North Carolina if that’s what it takes. He is already in the VA system, and is seen by doctors on a not so regular basis, as appointment are about 3 months apart. Any help would be greatly appreciated.
I don’t even know why this is in my Email….Since i was diagnosed with the AAA, back in 2016, further exams and medical records determined that i may have had the condition as far back since 2004, but it went undetected, either though i was going to the ER, from 2- 3 times a year!…and the condition was misdiagnosed as a mild heart attack….to this day i have yet to recieve the proper medications to prevent the stress and pain of the ailment…so i’m not impressed by the report, its only meant for the very few…and apparently i’m not one of them!..to cut down on the stress?…i stopped going to my appointments, what’s the point of going to the doctors, only to have the condition monitored, but not treated?
I am not a Veteran but my husband is and I went in and read on this valve after refilling his scripts. I have aortic stenosis and I have to get my valve replaced on March 19th. I don’t know what type my cardiologist is going to use but this is a very interesting article and I am going to print it off and see if this may be what he will be using. I have my pre-op next Friday so I’m going to find out what one he is going to use and show them this article.