Milwaukee Army Veteran Gerry Clemens was taking his dog for a walk four months ago when he had a heart attack. So, Clemens walked home and drove to urgent care.
A clinical evaluation revealed the severity of the situation, and he was transported to a local hospital where doctors determined he needed a heart transplant. However, his insurance wouldn’t fully cover the procedure.
Clemens had long believed that he didn’t qualify for VA benefits. However, as his family reviewed all possible options for covering the cost of the procedure, they discovered he was eligible for VA health care.
After he was enrolled, Clemens was transferred to the Madison VA.
“We then began an evaluation to determine whether or not he was a candidate for a heart transplant, and that then led to testing to see if he had been exposed to COVID-19,” said Dr. David Murray, medical director for Heart Failure and Transplant.
The routine test was positive, which meant recovery and six weeks of quarantine before they could attempt the surgery.
“There was just hurdle after hurdle after hurdle that he needed to overcome,” said Dr. Amy Fiedler, chief of Cardiac Surgery.
How would COVID-19 affect a transplant?
There were a lot of unknowns as to how the coronavirus would affect a transplant.
“That’s a big question mark for us right now specifically with respect to transplant,” said Fiedler, “because these patients require immuno-suppression after they receive the organ.”
In addition to his heart issues, Clemens also had pneumonia and issues with his kidneys.
“There were a number of not only medical, but psychological obstacles that he needed to overcome, being someone who was critically ill in the time of a pandemic,” said Fiedler.
Alone in his hospital room by himself day after day, Clemens received excellent care from the VA doctors and nurses, which improved his health to the point where he would be eligible for transplant.
The infectious disease consultants at the hospital determined and judged that the chance of reactivation of COVID-19 on the immune-suppression drugs would be very low, so the transplant team felt comfortable putting him on the transplant list.
“You’ve got to get well enough to get on a transfer list,” Clemens said, “and then they approved me for transplant.”
As a large man with an uncommon blood type, Clemens expected it would take months to find a compatible heart. “Two days later, they found the heart. So, it was like somebody was watching out for me,” he said.

Clemens is discharged following a long stay which included overcoming COVID-19 and a heart transplant.
Hard to believe I have his heart in my body
Still, Clemens found the prospect of a heart transplant was a lot to take in. “It’s hard to get your mind around it. A dead man saves your life. So many hours later I have his heart in my body. It’s hard to believe.”
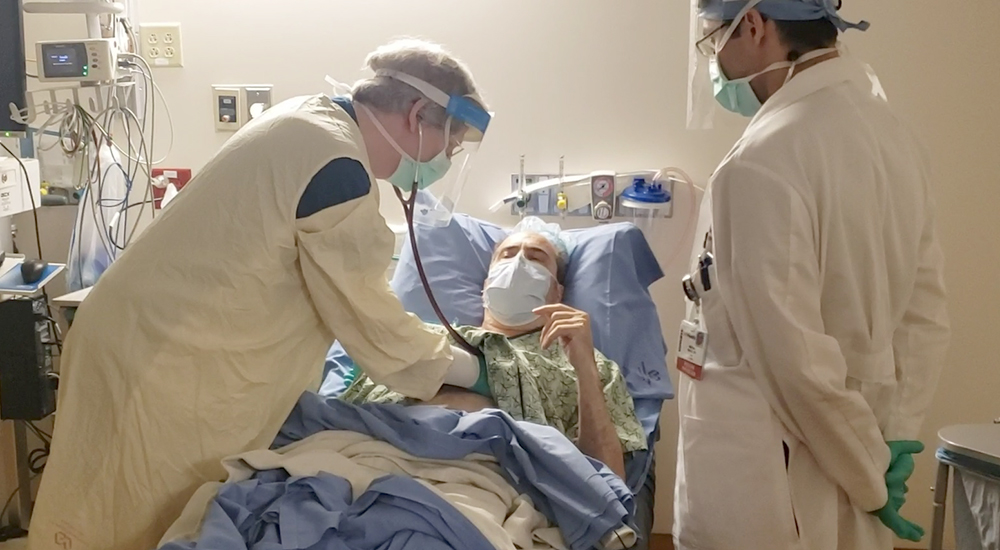
Pictured above, Clemens was evaluated by doctors at the William S. Middleton Memorial Veterans Hospital following his transplant.
Registered Nurse Abbey Vadnais saw the change immediately. Before the surgery it was evident to her how tired he was.
“If your heart isn’t able to profuse you entirely, it’s very fatiguing. For him, you could just see the light come back into his eyes.”
Dr. Fiedler was not surprised by the visible change.
“These Veterans are fighters. It’s a lot to go through to live with heart failure and to feel kind of lousy every day. Coupled with his long hospitalization before the transplant, it’s just amazing how much better he’s feeling with the new heart.
“Someone who saw him before the transplant and someone who saw him after the transplant can really see his spirit coming through now that he has a good working organ.”
First for procedure at Madison VA or University of Wisconsin Hospital
Clemens is the first patient at either the Madison VA or the University of Wisconsin Hospital to have a transplant following a successful recovery from COVID-19.
As a National VA Transplant Program, Veterans from across the country have access to this critical care through the Madison VA.
“No matter where they may live,” said Dr. Fiedler. “We’re happy to have them here and to evaluate them for transplant candidacy.”
“Everything is excellent, everything is top notch,” Clemens added. “I would recommend this place to anybody.”
Currently an outpatient, he will be a frequent visitor at the Madison VA over the next year as he regains his strength through physical therapy and doctors monitor his new heart.
Paul Rickert is chief of community relations/PAO and Greg Willenbucher is a program specialist at the William S. Middleton Memorial Veterans Hospital.
Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.