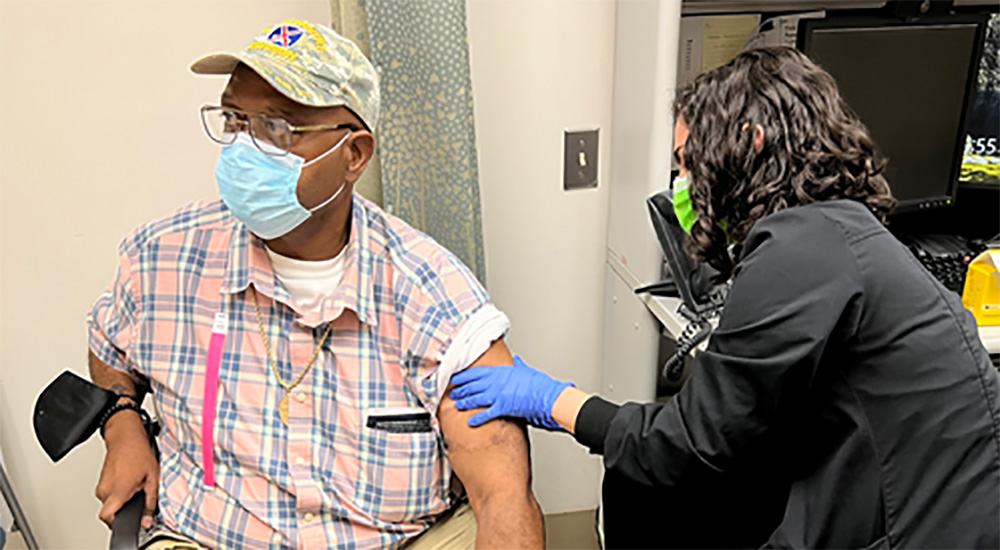
Army Veteran Waldence Cohen was diagnosed with diabetes in 2018. To help better track his blood sugar levels, he recently had a continuous glucose monitor (GCM) placed in his left arm.
“I started coming to VA for diabetic care a few years ago,” Cohen said. “The doctors here have been good to me and helped me get my numbers under control.”
CGM automatically tracks blood glucose levels (blood sugar) on a 24/7 basis. Tracking blood sugar levels continuously helps patients with type 1 and type 2 diabetes prevent diabetes complications. According to the CDC, these complications include heart attack, stroke, kidney disease and blindness.

According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), CGM works through a tiny sensor inserted under the skin, usually on the arm or abdominal area. The sensor measures the interstitial glucose level, the glucose found between cells. The sensor sends information wirelessly to the patients’ smartphone or tablet. If medical staff place the CGM with an insulin pump, the CGM can track data that can help determine how much insulin to administer.
Patients benefit from Artificial Pancreas System
“Since 2018, many of our patients have also benefited from the development of an artificial pancreas system,” said Dr. Julio Leey, director of the Diabetes Clinic at Malcom Randall VA. “This is an insulin infusion pump plus a glucose sensor (CGM). It results in the automatic adjustment of insulin to improve glucose control.”
To increase Veteran access to quality diabetic care, the Office of Rural Health has provided the funding necessary to implement these continuous glucose monitoring programs in VA Community Based Outpatient Clinics (CBOCs).
“VA has a unique advantage. Every clinic is staffed with a pharmacist and a dietitian who are both certified diabetes educators,” said Dr. Leey. “We are using advanced technology and educational outreach to improve the quality of care for Veterans both at the specialized clinics and the local level.”
The diabetic clinic at Malcom Randall VA is multifaceted. Its clinicians focus not only on diabetic care but also on patients’ nutritional needs, physical health and mental well-being. In the future, the clinic will be taking a closer look at the effects of depression on diabetic care and management.
“Without VA, I don’t know where I would be medically or financially,” said Cohen, after receiving his CGM sensor. “I’m a living testimony that it works.”
Veterans with type 1 or type 2 diabetes should consult their primary care physician or endocrinologist to determine if CGM sensor technology or the artificial pancreas system is right for them.
Topics in this story
More Stories
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.
In a decentralized clinical trial, Veterans can participate from their own homes or local VA instead of having to travel to a research site.






I highly recommend Medicare with Tricare for Life if you’re retired military and 65 or more.
It’s a joke, I’m a 100% disabled veteran & the care I get from the El Centro, California, VA outpost is the worst! I’ve given up fighting, I have Congestive heart failure, diabetes #2, Arrythima, left ventricular Block, multiple disc ruptures in my back, severe Arthritis & I’m 81 years old! Especially my prescriptions,!I pay for 1/2 of them with private insurance, although the VA is supposed to pay 100% of them! Sometimes they are 3, 4 weeks delivering my pain & other meds! It’s a mess! I’m stuck out in Salton City, Ca. 92275! My maternal cousin goes to Wilshire Branch in Los Angeles, California & receives great treatment & they are 100 times larger facility!
Why are veterans told we don’t qualify for cgm but an illegal on medicaid #oes?
My blood pressure machine is not reading my blood pressure correctly, can get another machine from the VA?
The va should allow newer diabetes type 2 medications to be used.
Keep going !