A lot has changed since Sec. Bob McDonald took over the reins at VA a little more than a year ago, yet the hard work to move VA forward continues every day.
Under Sec. McDonald, VA has taken a number of steps to strengthen accountability. Read more here. The department has also made progress to improve service for Veterans. You can read about that here. Since Aug. 7, 2014, when the Veterans Access, Choice and Accountability Act of 2014 (VACAA), was signed, VA has leveraged the law to enhance its health care system and improve service delivery to better serve Veterans. Read about that here.
Here are 19 reasons why VA not only turned the corner on last year’s crisis, but is moving forward to better serve Veterans.
1. Increasing Veterans’ access to health care appointments
In June 2015, VA completed 97 percent of appointments within 30 days of the Veteran’s preferred date, 93 percent within 14 days; 88 percent within 7 days. VA has completed 12 million same-day appointments, which is 20 percent of VA’s total appointments per year. VA also increased VA authorizations for care in the community, including the Choice Program, by 44 percent.
 2. Increasing transparency and accountability
2. Increasing transparency and accountability
VA began publicly posting patient access data online in June 2014. VA provides this access-to-care information to Veterans and the public knowing that transparency and accountability would help improve care for Veterans over time. Regularly updated patient access data is available for all VA medical centers and community-based outpatient clinics including average wait times, number of patients waiting for a scheduled appointment and number of patients that cannot be scheduled for an appointment in 90 days or less. Both completed and pending appointment data is available.
3. Improving customer service Veterans proud to call VA their own
VA continues its work to reorganize the department for success, guided by ideas and initiatives from Veterans, employees, and all of our shareholders. This reorganization is part of the MyVA initiative and is designed to provide Veterans with a seamless, integrated and responsive customer service experience. The MyVA Implementation Plan serves as a framework for achieving this transformation.
4. Training the nation’s health care providers
Whether you receive care in VA or not, there is a good chance that your healthcare provider received at least some of their clinical training in the Department of Veterans Affairs. VA trains 120,000 healthcare professionals per year, more than any system in the nation. An estimated 70 percent of all U.S. doctors have trained with VA.
5. Expanding care for victims of sexual trauma
Under authority from VACAA, VA expanded eligibility for Veterans in need of mental health care due to military sexual trauma (MST).
This expansion, which primarily pertains to Reservists and National Guard members participating in weekend drill, gives the authority to offer Veterans the appropriate care and services needed to treat conditions resulting from MST that occurred during a period of inactive duty training.
“VA simply must be an organization that provides comprehensive care for all Veterans dealing with the effects of military sexual trauma,” Sec. Bob McDonald said. “Our range of services for MST-related experiences is constantly being reexamined to best meet the needs of our Veterans.”
6. Ending the claims backlog
The claims backlog has been reduced from peak of 611,000 in March 2013 to 110,025 this week, an 82 percent reduction in 28 months. Claim-level accuracy increased from 83 percent in 2011 to 91 percent – issue-level accuracy is 96 percent.
Editor’s note: As of Oct. 3, the number of claims awaiting a decision for more than 125 days is down to 72,623.

Source: VBA Monday Morning Workload Report
7. Working with state and local partners to end homelessness among Veterans
On Jan. 28, 2015, Secretary McDonald and attorneys representing homeless Veterans in Los Angeles announced an historic agreement that dedicates the West Los Angeles VA campus to serving Veterans in need. VA published a written Veteran homelessness strategy and action plan for Greater Los Angeles on Feb.13, 2015, with the goal of ending Veteran homelessness in Greater Los Angeles by the end of the year. A new master plan for VA’s West Los Angeles campus will be completed by Oct. 16, 2015.
In the past year, the Mayors Challenge to End Veteran Homelessness, launched by First Lady Michelle Obama, has proven to be a game-changer as more than 700 local elected leaders have signed on to take action. States and local communities, such as New Orleans, are working with local Veterans Affairs offices to identify gaps in resources and driving the efforts to fill those gaps. These partnerships work. Since the 2010 rollout of the first-ever federal strategic plan to prevent and end homelessness and the January 2014 point-in-time homeless count, homelessness among Veterans nationwide has been slashed by one-third.

Ron Olson and VA Sec. Bob McDonald sign a historic agreement that dedicates the West LA Medical Center campus to serving Veterans in need
8. Helping the fastest growing group of Veterans — women.
VA Women’s Health Research Network (WHRN) is designed to increase inclusion of women Veterans in VA research, making sure women equitably benefit from VA’s investment in health care research. WHRN educates researchers about methods for including women, analyzing study results by gender and making it easier to recruit women.
9. Recruiting and hiring to provide more access to care for Veterans
VA has increased recruiting and hiring, bringing on more than 41,000 new employees over the last year with a net increase of over 12,000 medical professionals – a 4.15 percent increase. This includes 1,170 physicians, 4,113 nurses and 4,661 other select critical occupations.
VA has also increased salaries for physicians and dentists to close the pay gap with the private sector and to make retain professionals and make VA an employer of choice.
10. Funding $1.8 billion in promising research
During fiscal year 2015, nearly 3,400 VA researchers will work on more than 2,200 projects, with funding of more than $1.8 billion. One research study at the James A. Haley VA Medical Center in Tampa is looking into therapies to halt and possibly reverse Alzheimer’s progression. Another study focuses on whether mild traumatic brain injury, or TBI, may cause early brain aging.
11. Making a difference through volunteering
Sec. Bob McDonald launched VA’s Summer of Service volunteer initiative to “[turn] the spotlight on VA volunteers to thank them for the work they do and to show others how they can help as well,”
Community by community, state by state, VA invited the public to work together to serve Veterans. And they did. Volunteers are spending time at VA facilities and serving Veterans are making a difference.
12. Ending MRSA in VA healthcare facilities
In comparison to other hospital systems, VA is making great strides in reducing one of the most significant causes of healthcare-associated infections — methicillin-resistant Staphylococcus aureus, or MRSA. Within five years, healthcare-associated MRSA infections declined 69 percent in VA
13. Redefining the mission for disabled Veterans
VA funds $8 million in grants for adaptive sports. Grants are available to non-federal entities with experience in managing a large-scale adaptive sports program for persons with certain disabilities. The grants call for planning, developing, managing and implementing appropriate adaptive sports activities geared to disabled Veterans and Servicemembers. Adaptive sports are those that have been adapted or created specifically for people with disabilities.
14. Leading the way in mobile medicine, telehealth
Last year, VA launched several pilots of secure mobile applications to help Veterans, caregivers and VA clinical teams provide unprecedented opportunities and become active partners in health care through mobile technology. The driving force behind those initiatives is VA’s co-director of Connected Health, Kathleen L. Frisbee, MPH, Ph.D., who was named as one of the Top-10 influential women in health IT by FierceHealthIT for 2014.
VA is also national leader in telehealth services, which are critical to expanding access to VA care. Veterans use telehealth. At the end of FY2014, 12.7 percent of all Veterans enrolled for VA care received telehealth-based care. That’s over 2 million telehealth visits, touching 700,000 Veterans.
15. Changing lives through the GI Bill
For more than 70 years, VA has made the transition from service to society easier for Veterans through the GI Bill. Over 21 million home loans have been guaranteed by VA since 1944 as part of the original “GI Bill.”
Since the inception of the Post-9/11 GI Bill in 2009, more than $50 billion has been paid to more than 1.4 million Veterans and their dependents. In FY14, VA guaranteed 440,000 home loans totaling $100 billion, while also helping 80,000 Veterans avoid foreclosure, saving taxpayers over $2.7 billion. VA has maintained the lowest foreclosure rate (1.4 percent) in the industry for 25 of the last 27 consecutive quarters when compared to all other types of home loans.
One of the newest GI Bill benefits, the Fry Scholarship, was expanded this year under the Choice Act to serve spouses of fallen Servicemembers and processed nearly 4,000 applications in just the first eight months
16. Reaching out to Veterans in the community, on the road
VA’s 300 Vet Centers provide community-based counseling and a wide range of social and psychological services including professional readjustment counseling to Veterans and active duty Servicemembers (including members of the National Guard and Reserve components) and their families. The important work Vet Centers do was highlighted this spring by the White House’s Joining Forces initiative.
If a Veteran can’t get to a Vet Center, it’s possible a Mobile Vet Center, can get to them. These RV-style mobile clinics provide Veterans with vital, on-the-spot treatment and resources.
VA deployed a Mobile Vet Center and clinical staff in January to provide counseling services to Veterans, Servicemembers, families and fellow VA staff members in the wake of a shooting at Ft. Bliss, Texas.
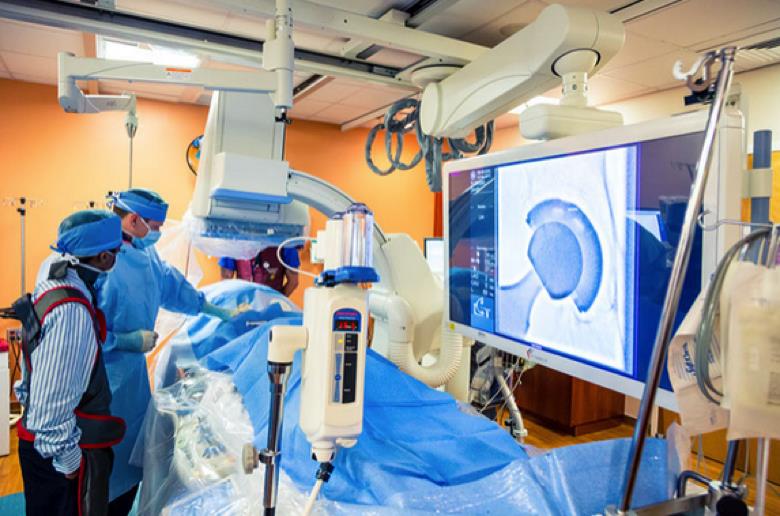
17. Using cutting-edge, personalized innovations to help Veterans
The Functional Electrical Stimulation Hand Glove 200 is a prototype device that incorporates both active functional electrical stimulation and passive robotic bio-mechanic movement. This combination is the first of its kind in hand and upper extremity rehabilitation. The Hand Glove actually allows the user to complete a full-length therapy session in spite of early muscle exhaustion. This may provide more rapid gain in strength and functional muscle mass.
The VA Innovation Creation Series aims to accelerate the development of personalized technologies to improve care and quality of life for Veterans. Recently, the VA Center for Innovation held its first ever “make-a-thon” at the Hunter Holmes McGuire VA Medical Center in Richmond, Va. At the event, Veterans explained everyday problems they face with missing limbs. The makers – students and engineers – then spent two days brainstorming design ideas and using 3D printers to manufacture prototypes in a competition. The results were “game-changing.”
18. Giving Veterans an artistic outlet at National Veterans Creative Arts Competition
The 2015 National Veterans Creative Arts Competition began on Jan. 1. During the months of January, February and March, Veterans enrolled at VA medical facilities or outpatient clinics were invited to enter their art, music, dance, drama and creative writing entries into the local competition phase. It’s an exciting time with art exhibits and performances by Veterans occurring across the country. At most facilities, the general public is invited to view the art and watch the performances, having the opportunity to learn about the arts as therapy and congratulate the Veterans for their artistic achievements.
19. Continuing to change Veterans’ lives through research
Two VA researchers received a coveted service award for ground-breaking work with paralyzed Veterans. For more than 25 years, Bill Bauman and Ann Spungen have worked together to make the lives of paralyzed Veterans better. Their dedication to their patients at the James J. Peters VA Medical Center in the Bronx was recognized as the pair was awarded the Samuel J. Heyman Service to America Science and Environment Medal.
Bauman and Spungen’s research focused on understanding the effects spinal cord injuries have on the human body. Eventually, they were able to attribute illnesses, like increased heart disease and asthma-like lung conditions, to high levels of paralysis. Once they were able to find the root causes of the conditions affecting their patients, Bauman and Spungen were able to create treatment plans for Veterans across VA’s healthcare system.
Reynaldo Leal contributed to this article.
Topics in this story
More Stories
Seven U.S. Army soldiers, one Army Reserve soldier and two Veterans are representing Team USA at the 2024 Olympic Games in Paris, which begins today.
The findings of this new MVP study underscore the importance and positive impact of diverse representation in genetic research, paving the way for significant advances in health care tailored to Veteran population-specific needs.
VA reduces complexity for Veterans, beneficiaries, and caregivers signing in to VA.gov, VA’s official mobile app, and other VA online services while continuing to secure Veteran data.













I am hoping someone can help me. I have been trying to get help for PTSD/MST. At my local VA, the wait list for weekly therapy sessions is greater than 30 days, and I am eligible for the Choice Program. The VA stated they will not give me a referral to the Choice Program. They told me to go to a Vet center, but (I am also eligible for travel reimbursement) but Vet Centers do not offer travel reimbursement. Is it legal for the VA to deny me using the Choice Program since my wait is longer than 30 days? I am a bit suspicious of this VA clinic…they are noyt even making appointments for veterans on the ‘wait list’. They are keeping a separate list. It does appear they are doing this to make their wait time stats look better. Thank you anyone for any help you can give. Sincerely, Hope E Ransom, disabled veteran, USAF
I lived in Prescott Valley but i used all my Medical Care and my Mental Health issues at the Prescott, Arizona Veterans Medical Center my comment is this how come a Veteran Patient Adocate can tell you say verbally but won’t write it down for you and if you change your Veteran Primary Care Doctor for a reason it does not show why in your Veteran Medical Records. ……..Please reply back. ….Thanks
I am from Memphis…My issue with my local VA is: If u call and do not know your extension, nobody answers the phone.. 901.523.8990…press 0..#2 Out of three reps …only one on duty..I was there at 8am …next available appointment was 11:30…left a message for him to call me..wed. His has not returned my call …today is Friday.
I have a couple of questions and one issue I need to address. Driving back is not an option..Thanks
I really like the VA as my Primary Care Provider, but I have a problem understanding why my Comp Exam for Depression/Anxiety was outsourced to a hospital in Yankton, SD and after completion I was told I should get benefits.
Then suddenly the VA at Sioux Falls said they wanted their our exam. I filed in May, it is August and my new appointment is the 24th. Wonder if I need a lawyer, I feel the VA does not want me to go to 100% just to save money.
Garry, I am just another disabled vet determined to help my brothers and sisters. If I may, I suggest you contact DAV an/or your Veteran Service Officer; both are a lot cheaper than a lawyer (free), & I personally have had great experiences with them. Good luck, my brother, & your name will be lifted up to the Creator as soon as this is sent!
Long Story Short– May 8, 2015, diagnosed with double vision, needed MRI. Couldn’t get MRI until July 23.. JUST a LITTLE over 30 days, huh??? Finally had the MRI, and the doc called with results the next day– “we found two tumors or cysts in your head. We want you to have ANOTHER MRI, more blood work and to see endocrinology.” That was the extent of the conversation!!!!!!!
My appointment wait was too long.
Doc has NO ‘bedside manner’
STILL waiting for appt with endocrinology, even though the doc said it needed to be done asap.
And MAYBE, do you think SOMEONE could call and explain to me about these tumors or cysts in my head so I know what’s wrong with me??????????? Not even my primary care doc has called..
Patti, If you can, go online & set up your “My Healthy Vet” acct. It can be a hassle, & at times really aggravates my PTSD, but you can get some good info. Your local/nearest clinic should have a “my healthy vet” rep; call & check it out.
FYI: When I read abt brothers & sisters that are hurting, I type, send, then pray. I am Cherokee indian & Irish, & will now lift your name to the Creator. I will pray for physical & emotional peace for you today.
Respect & Brotherly love
Fire Owl
The veterans choice card is worthiness in michigan,Va won’t do anything about it
To George Secord. Make sure your Non-Va dentist faxes all of your records, with the bill to your non-VA representative, and not to the dental office at the VA. Non-Va claims will not be paid without the non-VA medical/dental records.
I have not detected any change in the attitude of the bulk of local VA employees. Maybe they care about providing better care for veterans, and I just have not seen it. The telephone switch board at my local VA is a nightmare as opposed to actually getting any help. I was placed on fee basis after an untold number of cancelled dental appointments over a two year period, now the civilian dentist has not yet been paid after VA has had the bill over three months. The system is still not working as well as it could.
Why can’t I get health care at signoella naval base in sicily.
I am 100% disabled from agent orange.cant get meds or health care why
Yeah, well they really screwed up our VA. We are having so much trouble it’s pathetic. We had one of the best now it sucks. It has been since may and my husband is still waiting for an appointment for Neurology or spine doctor. The Health net set him up for a Dr. in our hometown and the dr. called a day before the appointment and said they don’t except the insurance. Now we are waiting for them to find another Dr. Never had any problems before they started fixing things.
VETERANS OF THE NEW LINCOLN VETERANS MEMORIAL VA HEALTHBEARS agree. We must politely convince Congress to properly fund our VA and cease an argument that has allready cost far too many lives
Talk to your local VET Center for help with PTSD. Talk to a patient advocate at the VA. Talk to your VAs homeless coordinator. Don’t let one bad egg ruin the VA for you. They have other employees. Keep reaching out and trying, be polite, don’t give up and don’t let one person anger you and steal your peace of mind. You are incharge of your peace and your treatment. Asking for help is one of the hardest things you’ll ever do. I’m grateful for your service and proud of you for reaching out!
My comments are getting them but what I’m saying is that if somebody doesn’t get a hold of assumed that I might be dead because the VA is not helping PTSD I’m not getting my psychiatrist help because because they will not make appointments for me they refused to see me they will not find me an ass I take archers the psychologist that we were going with insulted my wife and made her cry last made my wife break down and cry he was very rude condescending and very very fun and Carrie at the time of our homelessness at that time I refused to see him anymore and I refused to help me and I’m suffering from PTSD and it’s not getting any better my name is Dave my email is dave_hammit@yahoo.com hopefully someone will see these messages and try to get a hold of me my my phone number is on on the log on my on my sheet if you need to get a hold of me or you can email me and I will return the call please help help !!!
Mr. Hamit,
We asked VHA’s client relations team to reach out to you. If you need further assistance, please do not hesitate to contact us.
VAntage Point is monitored Monday through Friday during normal business hours. Any Veteran in crisis should contact the Veterans Crisis Line:1-800-273-8255 (Press 1) 24 hours a day, seven days a week.
Last summer we became homeless the VA has done very little to help us my wife was insulted by my psychiatrist this they will not provide psychiatric help for me and I’m suffering from PTSD late they’re willing to send me to an outside psychiatrist or psychologist that is over 42 miles away from my home my disability ratings went from 40% to 60% I am now disputing that because I’m in a wheelchair I need help nobody tells me I contacted sierra pacific Sierra I G office out here on the West Coast because Fresno is not helping me they get a little bit a help but nobody does any follow up if you’d like to get in touch with me my number is on it on my records in my email is dave_hammit@yahoo.com I’m hoping some One will contact us and get me some help before I die because that’s about the way it’s Hattie !!!
The beginning of last summer me and my wife became homeless the VA stop my mental health my percentage in my VA went from 40 to 60% but I’m getting little or no help from the VA I have called the Sierra Pacific IG out here in California and I did very little they want me to travel over 42 miles to see a psychiatrist because the one that I was seeing insulted my wife and made her break down and cry the VA is to do nothing but Dishon me I called the patient advocate Michael and I try I try to get a hold of Fresno VA directors office and they will not even talk to us they do not have they do not have an open door policy if you’d like to talk to me I have a phone number you can reach me through my email and Dave_hammit@yahoo.comi‘m hoping somebody will contact me before something drastic happens to me like death !!!
Great news, improvements are happening. But (and don’t you just hate the ‘but” . . . ) in all the blogs and posts where I read about vet’s problems with access to the VA etc I NEVER see a response from the VA. Why is that so?
Bob Sloan
Seaspray, Victoria
Australia
USAF 1966 – 1969
Mr. Sloan, I a 100% service-connected disabled vet, & would like to thank you for caring about us. I have seen answers to some posts on this blog; in fact, as I look a couple of comments above yours, there are 2 that are “hilighted” in blue frames, these are the replies.
I support Secretary McDonald, & believe he is working his tail-end off to improve & enrich the lives of ALL American veterans, afterall, he is our Brother-in-Arms.
THANK YOU AGAIN FOR YOUR SUPPORT!
I should have noted that some, not all, of these replies actually do come from VETERANS Administration staff. I have questioned a couple of them, & know this personally. Also, would like to let you know that the V.A. Secretary, Robert McDonald has made his email address public on a couple of occasions, & that he & I have exchanged several, normally non-VA-related emails.
God bless our troops, God bless our veterans, & may God bless America!
In fact, I pray the Creator will send His Great Spirit to ALL corners of the world, so that all He created may have a moment of peace today!
You all are doing a great job. I have been using the VA Hospital at Bay Pines with excellent care provided by everyone. I spent the majority of my career at Ft. Bragg which has a major Military Health Facility and Bay Pines matches them on the quality of service. I may add this is after going to Bay Pines routinely for 12 years so thanks again. Job well done and I have complete faith with Mr. McDonald. I have watched him on CSPAN appearing before both the House & Senate Veterans and Armed Services Committee’s. Right man for the right job, God bless him for volunteering. A millionaire I’m sure that did not have to get involved. He is an outstanding example of professionalism and selfless service. 10% of the VA maybe some bad apples but 90 plus % are doing a great service for us. I did 30 years in the Army and retired as a Sergeant Major. So i have been at the bottom of heap and up to the top and have a general view of how things are. Thanks again. Gary Mohler
P.S., I was in Special Forces and Special Operations and his comment to start a dialogue, that whoever misconstrued is nothing. I also consider his service in the 82nd as special forces too, the are Airborne. So that alone makes them special.
The press or whoever made a big deal of nothing! More spin or effort to spin stuff from the media. NO BIG DEAL!
I am having surgery for carotid artery stenosis. I have a choice card but when I called the VA for authorization I was told that I have to go to my VA medical center. My surgery is already scheduled for 08/31/15 at a non VA facility. I cannot wait on the VA and the VA hospital is more then 40 miles away. Can you help with my problem. Pleas reply to my email address. Thank you.
First of all let me say thank God for the VA they have been a virtual life saver for my husband and I. Yes you are hiring more people but have no where for them to work. Here in Michigan I hear of employees working out of closets and sharing offices that are too small for one person. You need more space. You need to enlarge you building areas, Nurses don’t want to work for the VA, because the work load is so high. They worry if they make a mistake from being overworked – they loose big time. They can work elsewhere for more money and less stress from trying to do so much with so little. Most clinics here do not even have a Doctor – only a NP. I have heard guys tell me the VA will now give you that app’t. sooner, but then they call to reschedule it later. You have make improvments, but still have a long way to go.
Many good things are happening, just not as fast as underserved vets like or need.
Affordable dental care needed for many vets. Insurance does not mean affordability. Rules for dental care are too restrictive. Why get dental clearances for surgery when they can’t repair any problems, just fill in a box? Used services when homeless, time ran out before all needed services could be completed. Bad teeth linked to bad nutrition, and heart disease.
It’s been over a month since I called the va in Tampa when I was placed in the hospital for 6 days….i started receiving bills and my doctor hasn’t seen me so I been going to a outside doctor. I also have went to a real pain management and the got my pain levels are 5&6 from a 9&10 and still waiting for appt. I had a va doctor tell me I should seek pain management on the outside if you know what I mean…you can call me
You should call the Non-VA Care Coordination department to ask them why your bills have not been paid. Their phone number is (813) 903-4202 or (813) 903-4244. As for not seeing your doctor, you should call back and request an appointment. If you called a month ago and no one called you back, then someone misplaced your message or something. Be proactive in your care and make the calls today.
You should call the non VA care coordination office to discuss your billing issues. Their numbers are (813) 903-4202 and (813) 903-4244. Also, if you need to see your doctor and they haven’t made you an appointment, then you should keep calling until you get what you need. You can also seek the assistance of a patient advocate. Either way, take action and be proactive in your care. Don’t just give up and pay for the care of your own. And don’t expect them to reimburse you for the care you received on the outside. They usually won’t reimburse you for outside care if they didn’t refer you there to begin with.
Unhappy Vets are quick to complain, but you all are getting it right. You all are doing it better.
Question, why are dental services not offered except to limited specific terms? Quality affordable dental services are non existent in many areas. Teeth effect nutrition. Bad dental care has been linked to heart disease.
I know you all can find a solution to serve vets in this underserved population.
I was able to use dental services when I was homeless, but the time limit ran out before all needed services could be completed.
Thanks for letting me vent,
Klausihnenfeld
Dear Sir, I take offense to your comment that we are quick to complain! ONE EXAMPLE: The director of the Phoenix VETERANS Hospital made apx. $170K a year & rec’d a bonus of almost $10K in the same year that 40 veterans that facility was responsible for DIED! AT ONE FACILITY! A veteran who was lucky enough to live through the HELL they went through serving this great country, rated at 100%, gets ALMOST 1/3 of that bonus amt per month.
While I respect your right to free speech (that’s what we fight for), I also ask that you respect our same right. I do agree with you that there is TOO MUCH complaining, & NOT ENOUGH action. I have challenged all veterans to STAND UP FOR YOURSELVES; even published my email address, & got very little response. STOP COMPLAINING & WAITING FOR SOMEONE ELSE TO DO THINGS FOR YOU. VETERANS – UNITE & STAND UP FOR YOURSELVES !!!
dannyg55@centurylink.net
Please answer my letter you should have received on or about July 6 or 7. I have been treated like crap at the Jackson VA Medical Center. Wonder if anyone will write me or call.
John Busby, MSG E8, Retired US army, [Personal identifying information redacted]
They are not going to reply. You see where they spend the money. On the machine. Nothing for increasing disability payments for the veterans, and plenty of pay increases for doctors and staff. Why not give veterans what they truly deserve. A better life, and as much pay as they give a person on the cleaning crew at the VA offices.