Last winter Dr. Gilbert Teague began working with his VA facility’s team to implement the VA National TeleStroke Program. An army Veteran, Teague is chief of primary and specialty medicine at VA Black Hills Health Care System in Fort Meade, South Dakota.
Teague knew this innovation would improve care to many Veterans, especially in rural areas like the Black Hills, but he did not expect it to save his own life two months later.
Teague suffered a stroke on January 24. He lost motor and language function the moment his stroke began, falling motionless to the floor of his home. Teague’s wife called the ambulance, which transported him to the Fort Meade VA Medical Center where he works.
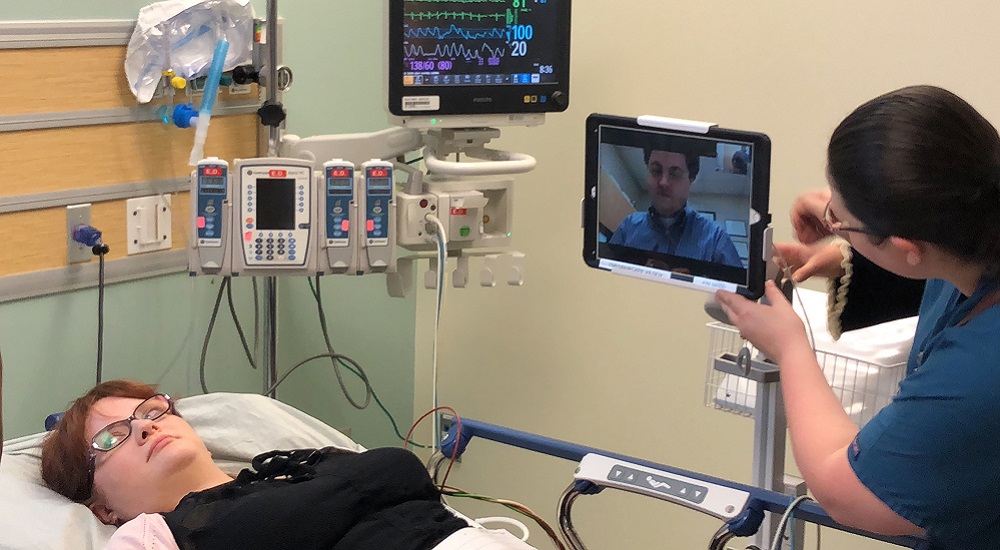
Upon his arrival at the facility, Dr. Peter Hasby, chief of staff, immediately recognized Teague’s symptoms as a stroke and called VA TeleStroke. The VA TeleStroke physician on duty, based in New Haven, Connecticut, connected to Teague and his onsite care team within minutes to examine him, review his medical history and brain imaging, and ultimately direct timely administration of the “clot-busting” medication alteplase.
“Studies show that people suffering a stroke may benefit from alteplase for up to four and a half hours following stroke onset. However, ‘time is brain’ and patients treated as soon as possible have the best chances for good recovery,” said Dr. Glenn Graham, VA deputy national director of neurology. “This places a burden on medical centers that lack the local expertise to make rapid decisions for acute stroke patients. TeleStroke enables subspecialists at large tertiary VA medical centers to provide care to Veterans at smaller VA facilities in a timely manner.”
VHA’s Office of Connected Care supplies the mobile tablets to VA facilities throughout the country that make remote tele-care possible. Connected Care partners with VHA’s Office of Rural Health on the VA National TeleStroke Program.
Teague noted there are two types of strokes, and both destroy brain tissue as time passes. Ischemic strokes are caused by blood clots, while hemorrhagic strokes are caused by bleeding into the brain. The first line of treatment against an ischemic stroke, alteplase, exacerbates hemorrhagic stroke bleeding, and cannot be administered until a hemorrhagic stroke is ruled out by brain imaging. Dr. Pooia Fattahi, a remote stroke specialist, diagnosed Teague with an ischemic stroke and recommended alteplase to break up his blood clot.
1.9 million brain cells die every minute treatment is delayed
Fattahi’s decision to administer alteplase bought Teague time to be flown to the Sioux Falls VA Health Care System for additional treatment, without significant damage to brain tissue. Dr. Sharyl Martini, medical director of the VA National TeleStroke Program, said if the Fort Meade facility did not have access to remote stroke specialists via Telehealth technology, the alteplase injection would have been delayed. Because each minute of delay results in death of an additional 1.9 million brain cells, that delay might have cost Teague his opportunity to recover fully and enjoy a high quality of life.
“TeleStroke leads the neurology community in emergency stroke treatments,” said Katherine Murphy, program manager in VA Specialty Care Services. “Through direct employment with the VA or through affiliation, specialists seek to work with innovative technology, and the chance to provide optimal care to our nation’s Veterans.”
By the time Teague arrived in Sioux Falls, his blood clot had dissolved significantly, and a much smaller section of his brain was affected.
“Even though I hope no one is ever in need of TeleStroke services again, I will always be glad we implemented TeleStroke in VA Black Hills,” said Teague, who has fully recovered from his stroke and has returned to work at Fort Meade VAMC to provide care to Veterans.
Here’s more information on VA Telehealth Services.

Topics in this story
More Stories
Seven U.S. Army soldiers, one Army Reserve soldier and two Veterans are representing Team USA at the 2024 Olympic Games in Paris, which begins today.
Study underscores important role COVID vaccination can have in protecting Veterans from infection and reducing long-term health consequences
Columbia VA’s robotic surgery teams completed their 800th robotic surgery and are on schedule to hit 1,000 by the end of the year.







Tell you what the way @DeptVetAffairs handled my fathers surgery id invest all the money i can into helping This program through approved supervised Programs! #NOMORESKIDROW #BATTLEFORLA #VETERENSUPPORT