VA researchers are exploring the best combinations of conventional and complementary treatments to treat chronic pain in Veterans. (Photo: ©iStock/vellena)
This article originally appeared in VA Research Quarterly Update.
Dr. Matthew Bair is a general internal medicine physician and VA health services researcher. He is a core investigator with the HSR&D Center for Health Information and Communication (CHIC) in Indianapolis. He is also an associate professor of medicine at Indiana University School of Medicine. His main research interest is pain management in primary care.
Over the last 15 years Bair has been part of a team that has worked to improve pain management for Veterans in primary care. In particularly, they have looked at combining pharmacologic (drug) and non-pharmacologic treatments.
VARQU spoke with Bair about his work to help Veterans better manage their chronic pain.
How prevalent is chronic pain in the Veteran population?
I think estimates for the prevalence of chronic pain in Veterans range from 50 percent in men to even higher in women Veterans. Dr. Robert Kerns and his team at West Haven, Connecticut, said that women Veterans have prevalence as high as 70 to 75 percent. At least one in two, or three out of four Veterans have chronic pain. That is higher than in the general population—about one in three people in the general population have chronic pain.
What are some of the unintended consequences of using opioid therapy?
Like any other pain treatment, the primary goals of opioid therapy are to reduce pain intensity and improve function. So if you take opioids away, there is the potential that you could actually increase pain intensity or worsen function.
I think there are also some associated issues that could potentially worsen quality of life. We know that patients with chronic pain and particularly patients on opioid therapy can be subject to stigmatization. I worry that if opioids are restricted significantly, that stigmatization could be heightened and, potentially, racial and ethnic disparities could widen. There is some data that suggests that opiates are less likely to be used in some clinical settings among African Americans relative to whites.
Besides opioid therapy, what evidence-based treatments are available to treat chronic pain?
There are multiple evidence-based treatments to treat chronic pain—opioids are just one, in terms of pharmacologic treatment. For example, non-steroidal anti-inflammatory drugs (like ibuprofen) are an evidence-based treatment for many chronic pain conditions, particularly osteoarthritis.
There are also many non-drug treatments that are evidence-based for the treatment of chronic pain. The strongest evidence is for cognitive behavioral therapy (CBT)—which is psychological therapy.
CBT provides patients with self-management strategies so they can better cope with their pain. It uses goal-setting, which is a helpful strategy to help patients improve their quality of life and function. Some patients have what we call maladaptive thoughts related to their chronic pain; in those cases, CBT tries to substitute those negative thoughts with more positive, more helpful, more adaptive thoughts to better cope with their pain.
Physical therapy interventions—particularly a tailored exercise program—are also evidence-based. We have the whole suite of cognitive and integrative health treatments that are growing not only in popularity, but in evidence, from acupuncture treatment to massage therapy to spinal manipulation therapy, chiropractic therapy, yoga-based therapies, or tai chi.
So that’s the good news. There are a lot of options to treat chronic pain. The downside is that each therapy individually has modest benefits. We don’t have a treatment that is knocking it out of the park in terms of effectiveness. So the challenge is for an individual patient to find the right treatment or treatments. Usually what we need to do to get a stronger treatment effect is to combine treatments. And that’s where I’m particularly interested: trying to find the right combination of pharmacologic treatment and non-pharmacologic treatment that improve treatment effects.
Tell us about some of your latest research.
I think we need to improve the evidence base for non-pharmacologic treatments, particularly in the complementary and integrative health area. We have an ongoing study that is looking at comparing yoga therapy versus a physical therapist-guided exercise program for Veterans with fibromyalgia. We are finishing up that trial.
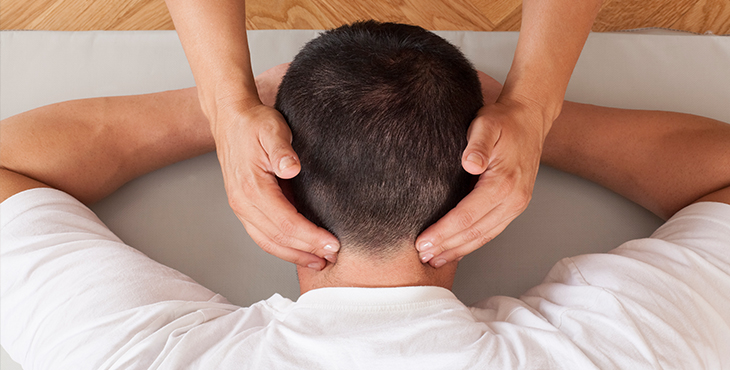
We also have an ongoing clinical trial that’s looking at Veterans with chronic neck pain, comparing two different types of massage interventions. One massage intervention is delivered by licensed massage therapists—what we view as the gold standard. We are comparing that to caregiver-delivered massage. Caregivers—spouses, children, or adult caregivers—will be trained in Swedish massage techniques so that they may apply them to Veterans with chronic neck pain.
I’m also interested in the overlap between chronic pain and PTSD and chronic pain and insomnia. Again, these are very common comorbidities—they go hand in hand. We see them a lot in patients with chronic pain, whether its anxiety symptoms, such as PTSD, or poor sleep, which can worsen their treatment response and worsen pain treatment outcomes. So we need to address those comorbidities.
To read more of this interview, click here to visit VA Research Quarterly Update.
Topics in this story
More Stories
Diverse representation of women in health care research allows MVP to make discoveries for women’s health
Join the Million Veteran Program online. You will have the option to receive an at-home blood sample collection kit in the mail.
VHA's new podcast series, New Horizons in Health, features a candid discussion of psychedelic assisted therapies for Veterans experiencing mental health conditions.






Do veterans have a common type of comorbidities, What can be done to minimize such cases?
How do I get in touch with the clinical trail for chronic neck pain?
Lawrence, you can go to this webpage and follow the directions to search for clinical trials on “chronic pain” https://www.research.va.gov/for_veterans/find_studies.cfm
Comorbidities are indeed common; the pain itself can lead to or exacerbate depression, insomnia and “feed off” PTSD symptoms as they do pain symptoms, exacerbating both. However, some of the methods being explored for treating the pain and/or other comorbidities are just as harmful as the opioids, perhaps more so for the longer term. For example, use of yoga, without fully informing patients as to what yoga actually is (it is NOT simply a nice exercise/stretching regimen), can, in fact, impact their immortal souls in a very negative way. Now, I know the VA doesn’t like to hear about immortal souls; but like it or not, they do not have a right to endanger anyone’s soul without full disclosure as to what the dangers of any practice are, the same as they don’t have a right to operate or do other procedures on any individual without a fully informed consent, and so far as I’ve seen at my local VA,that is NOT happening with spiritual practices such as yoga. I knew, and promptly rejected it as any course of “therapy” for my own pain, because I’d studied religions for decades before the problem arose and know what their practices are about, not just my own beliefs. But most do not, because they haven’t made a study of religions beyond their own beliefs, and aren’t aware of the danger into which the practice is placing them. It applies to Chi, Chakras, accupunture or accupressure, and a number of others. They are, in fact, worship practices, attached to various other deities. So while the VA is refusing to allow Christian worship in its facilities; it’s actually introducing and encouraging OTHER religious practices, also wrong.